VA Disability Ratings and Benefits for Respiratory Conditions

CCK Law: Our Vital Role in Veterans Law
Respiratory conditions are among the most common conditions for which veterans become service connected, particularly because of their association with military burn pit and Agent Orange exposure. Continue reading for a comprehensive look at the different types of respiratory conditions affecting veterans, how to become service connected for them, and how VA rates these conditions.
Service Connection for Respiratory Conditions
Service connection is the process veterans must go through for VA to recognize that a specific disability is related to their military service. Generally, there are three elements to service connection:
- A Currently Diagnosed Disability—There needs to be a medical condition or functional impairment that the veteran is experiencing. For respiratory conditions, the veteran will usually need to have a current diagnosis of a respiratory condition in order to file a claim for service connection.
- In-Service Event or Occurrence—In addition to a diagnosis, there needs to be an in-service event or occurrence which caused the veteran’s respiratory problem. This could be an exposure, such as exposure to burn pits, which caused or contributed to the respiratory condition that the veteran developed.
- Medical Nexus—The veteran will also need a medical nexus to link the their service with their respiratory condition. This usually requires medical evidence. This element could also be supplied by the presence of a presumption in VA’s regulations. VA does have some regulations that presume that certain conditions are related to in-service exposures.
Common Causes of Respiratory Conditions in Veterans
Burn Pits and the PACT Act
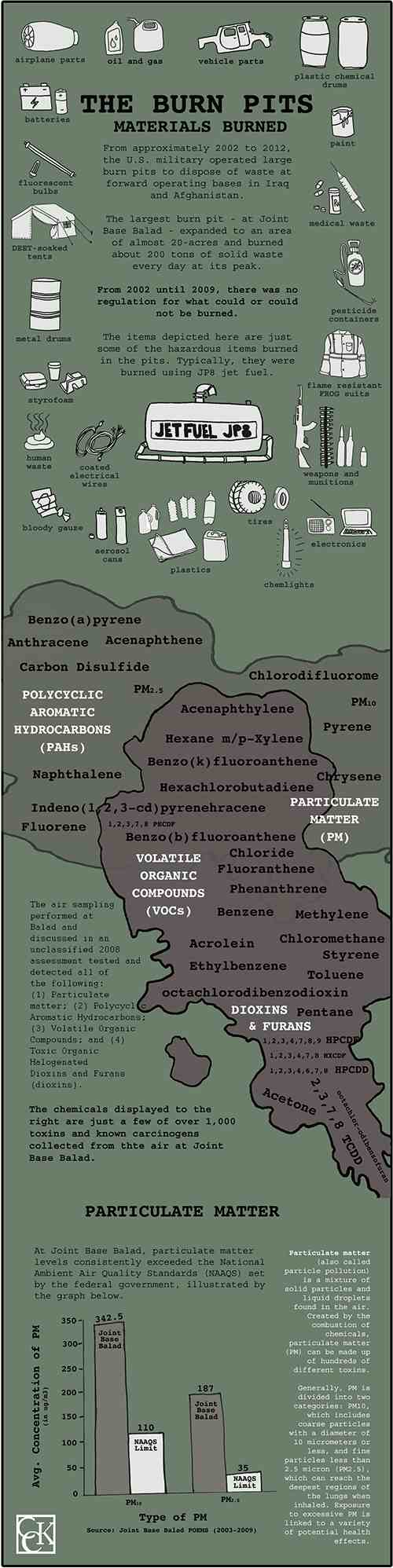
Military burn pits are large areas of land in which the military and its contractors incinerated all waste generated by military bases. The United States military used burn pits as part of its waste disposal protocol in places such as Iraq, Afghanistan, and Djbouti in the post-9/11 era. The practice was effective in reducing large quantities of waste, but the pits emitted plumes of toxic smoke which were later found to cause damaging health effects. Materials such as human and medical waste, plastic, rubber, petroleum, and ammunition were disposed of in burn pits.
Burning hazardous materials and chemicals in open-air pits emits toxic substances and carcinogens that can cause a host of diseases, some severe and even deadly. Specifically, respiratory conditions were caused by breathing in these toxic fumes.
As such, respiratory conditions, among other conditions, have been known to affect veterans of Operation Enduring Freedom (OEF) and Operation Iraqi Freedom (OIF).
Under the PACT Act, VA now recognizes many respiratory conditions as being connected to burn pit exposure. Veterans who served in the Middle East during the Gulf War or Global War on Terror and who went on to develop respiratory conditions may be eligible for presumptive service connection for those conditions.
Some of the respiratory conditions VA made presumptive under the PACT Act for burn pit exposure include:
- Asthma diagnosed after service
- Neck cancer (of any type)
- Respiratory cancer (of any type)
- Chronic bronchitis
- COPD
- Constrictive bronchiolitis or obliterative bronchiolitis
- Emphysema
- Chronic sinusitis
- Chronic rhinitis
- And more
Sulfur Mine Fire in Iraq
In June of 2003, a fire ignited at the Mishraq State Sulfur Mine Plant near Mosul in northern Iraq. The fire burned for almost a month, becoming the largest manmade sulfur fire in recorded history. It released roughly 42 million pounds of sulfur dioxide per day, as well as a significant amount of hydrogen sulfide.
Field samples of air in the vicinity of the fire detected these toxic gases at levels immediately dangerous to health and life. As such, servicemembers involved with fighting this fire were at risk for negative health-related outcomes.
Firefighters from the 101st Airborne Division were the most exposed as they were in closest proximity to the fire for the longest periods of time. As a result, they experienced both short-term and long-term health effects. Exposure to the toxins caused many respiratory health issues, such as lung damage.
Particulate Matter (PM) and Respiratory Conditions
Veterans who were stationed in Iraq or Afghanistan were likely exposed to dust, sandstorms, and other environmental hazards. The dust and other particles in the environment contained what is called particulate matter.
According to the EPA, particulate matter is a complex mixture made of extremely small particles and droplets. Particulate matter can be found in dust, sand, acids, organic chemicals, and even metals. Inhaling particulate matter can cause respiratory conditions and damage the lungs.
Oil Well Fires and Respiratory Conditions
During the Persian Gulf War, Iraqi military forces set fire to over 600 oil wells in Kuwait. These fires created a massive environmental hazard and burned for eight months. As a result, soot and dirt were released into the air and inhaled. Inhaling these hazards, especially over that long period of time, caused a host of serious respiratory issues.
MUCMI
Medically Unexplained Chronic Multisymptom Illnesses, or MUCMIs, affect Gulf War Veterans who served in Southwest Asia. These veterans, upon returning from service, began experiencing a number of unexplained illnesses and symptoms.
As a result, VA created a presumption under 38 CFR § 3.317 to make it easier for veterans to obtain service connection for these unexplained illnesses. In order to qualify for presumptive service connection, the veteran will typically need to have been actively serving in the military in Southwest Asia between August 1, 1990 and December 31, 2026.
Agent Orange Exposure and Respiratory Conditions
Agent Orange is one of several herbicides, sometimes referred to as “rainbow herbicides,” that were used during the Vietnam War era. The herbicides were used by the United States military to deforest large areas of land, interrupt enemy food supplies, increase visibility, and prevent ambush attacks against US service members. Many veterans came into contact with Agent Orange, including those who served in areas other than Vietnam.
Specifically, Agent Orange was a mixture of two different kinds of highly toxic chemicals: 2, 4-D and 2, 4, 5-T. The highly toxic dioxin contaminant known as 2, 3, 7, 8-TCDD is a byproduct that is produced by Agent Orange. Today, we are aware of the significant health effects related to herbicide exposure.
Like the presumptions described above, there is also a presumption of service connection for Vietnam War Veterans who were exposed to Agent Orange during their service. This presumption is not just limited to veterans who served boots-on-the-ground in Vietnam, however. It is also extended to Blue Water Navy Veterans, as well as veterans who served in certain locations in Thailand, Korea, and some additional places.
Veterans who have been presumed to have been exposed to Agent Orange may have developed certain respiratory cancers as a result of their exposure. These conditions may include cancers of the lung, bronchus, larynx, or trachea.
Compensation and Pension (C&P) Exams for Respiratory Conditions
Once a veteran files a claim for a respiratory condition, VA may request a Compensation and Pension exam, or C&P exam. To do this, VA may call the veteran or send a letter. It is very important to make sure VA has the most up-to-date contact information to ensure that the veteran does not miss any C&P exam requests. It is also very important to attend the exam, as failure to attend can result in VA denying the veteran’s claim.
The exam will usually be performed by a VA physician or a VA contracted physician. Before the exam, the examiner will review the veteran’s c-file. This will contain any documentation that has been previously submitted to VA, as well as the veteran’s medical and service records.
The veteran may also use a DBQ, or Disability Benefits Questionnaire, to bolster their claim. A Disability Benefits Questionnaire is a form created by VA that allows the veteran to address important aspects of their condition, such as symptoms, severity, and possible causes, as well as the relationship between their condition and other disabilities.
The veteran may also have their private doctor fill out a DBQ for them. This can be helpful, as the doctor who typically treats the veteran’s respiratory condition can speak to the specific details of their illness.
Understanding VA’s Key Measurements for Respiratory Conditions
To understand VA ratings for conditions such as Asthma and COPD, you must first understand the measurements VA uses to assess the severity of a respiratory condition.
- Forced Expiratory Volume in 1 Second (FEV-1) is the maximum amount of air that a person can breathe out in 1 second compared with the FEV-1 for a normal person of your size and age.
- Forced Vital Capacity (FVC) is the total amount of air that a person can exhale after taking a full breath in.
- VA uses a ratio of the two above metrics to determine severity as well.
- Diffusion Capacity of the Lung for Carbon Monoxide by the Single Breath Method (DLCO (SB)) measures the ability of a person’s lungs to transfer gas from air that is inhaled to their red blood cells by comparing carbon monoxide levels retained after exhaling.
- Exercise Testing determines how much oxygen a person’s blood uses when they are functioning at maximum capacity, measuring the maximum amount of physical activity that a veteran can repeat and sustain. Measurement is expressed by the amount of oxygen used by your body weight per minute.
- Pre-Bronchodilator vs. Post-Bronchodilator Spirometry is another test VA may use to measure lung function. This test measures a person’s capacity to breathe before and after administering a bronchodilating drug (e.g. albuterol) via inhaler. Depending on the results, this test could indicate conditions like asthma or COPD.
Veterans should also bear in mind that VA generally uses the examination results that are most favorable to the veteran’s claim when assigning a disability rating for a respiratory condition.
*It is important to note that other effects of respiratory conditions not listed in the rating schedules below are still relevant to your VA rating.

Most Common Respiratory Conditions and How VA Rates Them
Not all respiratory disabilities are rated the same, and some are eligible to receive a higher VA disability rating than others.
Importantly, veterans can only be rated for one respiratory condition, even if they suffer from multiple ones (e.g. if a veteran suffers from asthma, COPD, and sleep apnea). This is to prevent “pyramiding“, or veterans receiving multiple disability ratings for the same symptoms. Instead, VA will typically only evaluate the dominant respiratory disability and use that as the basis for the veteran’s rating.
Sleep Apnea—Diagnostic Code 6847
Sleep apnea is a potentially serious sleep disorder in which a person’s breathing is repeatedly interrupted during the course of the night. Sleep apnea must be diagnosed with a sleep study to qualify for service-connected compensation.
- 100%—Chronic respiratory failure with carbon dioxide retention, the need for tracheostomy, or cor pulmonale (enlargement or failure of the right side of the heart).
- 50%—Veteran requires the use of a breathing assistance device such as a CPAP machine
- 30%—Persistent daytime hypersomnolence (persistent daytime sleepiness that does not improve with sufficient sleep)
- 0%—Veteran’s condition is asymptomatic, but sleep disorder has been documented
Rhinitis—Diagnostic Code 6522
Generally speaking, allergic rhinitis is an allergic response to specific allergens (i.e., a substance that causes an allergic reaction). Specifically, symptoms tend to occur when you breathe in something you are allergic to, such as dust, animal dander, or pollen. Rhinitis is usually a temporary condition. To receive VA disability benefits, your rhinitis must be chronic.
- 30%—Veteran has polyps present
- 10%—No polyps are present, but greater than 50% obstruction of nasal passages on both sides of complete obstruction of one side.
Constrictive Bronchiolitis—Diagnostic Codes 6600-6604
Constrictive Bronchiolitis (CB) is a small airway fibrotic respiratory disease characterized by the inflammation of small airways. Sufferers of CB often have persistent cough and dyspnea.
CB is very difficult to diagnose and extremely uncommon. People with CB can have shortness of breath when they exert themselves, but also have normal chest X-rays and pulmonary functioning test results. CB is often diagnosed as chronic pulmonary obstructive disease (COPD).
To correctly diagnose CB, veterans must undergo a surgical lung biopsy, an invasive procedure that can confirm their diagnosis. Since CB is uncommon and difficult to diagnose, unfortunately, VA frequently rates veterans with this condition incorrectly.
This condition has affected many post-9/11 veterans and has been linked to veterans exposed to sulfur mine fires and burn pits.
- Per Training Letter 10-03, Constrictive Bronchiolitis is rated analogously to:
- Bronchitis
- Bronchiectasis
- Asthma
- Emphysema
- COPD
This condition must be given extraschedular consideration when the veteran’s constrictive bronchiolitis impacts their ability to work.
Asthma—Diagnostic Codes 6602
Asthma, also called bronchial asthma, is a respiratory condition in which a person’s airways become inflamed, making it difficult to breathe. When the airways become inflamed and narrow, some people may cough, wheeze, or experience shortness of breath. Severity ranges from person-to-person and can be minor or very severe.
100% Asthma VA Rating:
- FEV-1 less than 40% predicted; or
- FEV-1/FVC less than 40%; or
- More than one attack per week with episodes of respiratory failure; or
- Require daily use of systemic (oral or parenteral) high dose corticosteroids or immunosuppressive medications.
60% Asthma VA Rating:
- FEV-1 of 40 to 55% predicted; or
- FEV-1/FVC of 40 to 55%; or
- At least monthly visits to a physician for required care of exacerbations; or
- Intermittent (at least three per year) courses of systemic (oral or parenteral) corticosteroids.
30% Asthma VA Rating:
- FEV-1 of 56 to 70% predicted; or
- FEV-1/FVC of 56 to 70%; or
- Daily inhalational or oral bronchodilator therapy; or
- Inhalational anti-inflammatory medication.
10% Asthma VA Rating:
- FEV-1 of 71 to 80% predicted; or
- FEV-1/FVC of 71 to 80%; or
- Intermittent inhalational or oral bronchodilator therapy.

Chronic Obstructive Pulmonary Disease—Diagnostic Codes 6604
Chronic Obstructive Pulmonary Disease (COPD) is an inflammatory lung disease that causes obstructive airflow to and from the lungs. Symptoms of COPD include coughing, difficulty breathing, wheezing, tightness of the chest, and frequent respiratory infections. COPD is often referred to as chronic bronchitis or emphysema. However, a person can have symptoms of both, or, for example, have symptoms of COPD and not bronchitis.
100% COPD Rating:
- FEV-1 less than 40% predicted; or
- FEV-1/FVC less than 40%; or
- DLCO (SB) less than 40% predicted; or
- Maximum exercise capacity less than 15 ml/kg/min oxygen consumption; or
- Right heart failure; or
- Right ventricular hypertrophy; or
- Pulmonary hypertension shown by Echo or cardiac catheterization; or
- Episodes of acute respiratory failure; or
- Require outpatient oxygen therapy
60% COPD Rating:
- FEV-1 of 40 to 55% predicted, or;
- FEV-1/FVC of 40 to 55%, or; DLCO (SB) of 4 to 55% predicted, or;
- Maximum oxygen consumption of 15 to 20 ml/kg/min (with cardiorespiratory limit)
30% COPD Rating:
- FEV-1 of 56 to 70% predicted, or;
- FEV-1/FVC of 56 to 70%, or;
- DLCO (SB) of 56 to 65% predicted
10% COPD Rating:
- FEV-1 of 71 to 80% predicted; or
- FEV01/FVC of 71 to 80%; or
- DLCO (SB) of 66 to 80% predicted
TDIU and Respiratory Conditions
Veterans who are prevented from working because of a respiratory condition may be able to receive a monthly VA disability benefit called total disability based on individual unemployability, or TDIU. This benefit compensates veterans at the 100 percent rating level, even if their disability rating may be less than that.
There are generally two pathways to become eligible for TDIU:
- 38 CFR § 4.16a (“Schedular”)–For this form of TDIU, the veteran must have:
- One condition rated at minimum 60 percent OR
- two conditions that can be combined to reach 70 percent, where one condition is at minimum 40 percent
- 38 CFR § 4.16b (“Extraschedular”)–This form of TDIU is for veterans who may not be able to achieve the ratings necessary for schedular TDIU but are still unable to obtain substantially gainful employment on account of their conditions. In this instance, the veteran must prove that their condition uniquely hinders their ability to obtain substantially gainful employment and therefore should not be rated on the standard disability rating criteria.
Veterans with multiple conditions may have a combined rating which would make them eligible for TDIU. As a result, veterans who receive a rating for their respiratory condition may be able to receive compensation at the 100 percent rating level through TDIU.
Getting Assistance if Your Claim for a Respiratory Condition Has Been Denied
As claims for respiratory conditions are among the most commonly filed, they are also some of the most commonly denied. If your claim for a respiratory condition has been previously denied, the veteran’s disability team at Chisholm Chisholm & Kilpatrick LTD may be able to assist you. For more information, as well as a complimentary case review, contact us at (800)544-9144.
About the Author
Share this Post