VA Compensation for TBI and PTSD

CCK Law: Our Vital Role in Veterans Law
What Is a Traumatic Brain Injury (TBI)?
Traumatic brain injury (TBI) can be caused by many factors, but typically involves a blow to the head or an object penetrating the brain. TBI can result in brain dysfunction, but not always. A concussion is a common form of TBI.
Military service can place servicemembers at a higher risk for TBI than civilians. Common occurrences of TBI in the military can include:
- Combat exposure
- Motor vehicle accidents
- Personal assault
- Falls
Additionally, TBIs are considered a signature wound of the post-9/11 wars. This is likely due to the increased use of improvised explosive devices (IEDs) during these wars.
Diagnosing TBI
After suffering a TBI, symptoms may begin to manifest cognitively, physically, behaviorally, and/or emotionally. Symptoms, and residuals, commonly include:
- Dizziness and headaches
- Impaired vision or hearing loss (e.g., tinnitus)
- Weak muscles
- Stroke, seizures, or paralysis
- Coordination, balance, and gait disorders
- Difficulty with written and verbal communication
- Impaired memory and difficulty concentrating
- Depression
- Poor judgement
TBIs are initially diagnosed as mild, moderate, or severe based upon medical testing and the severity of the veteran’s symptoms. While mild brain injuries usually resolve themselves within about six months, there can be significant residuals associated with more severe TBIs.
How Is TBI Rated?
VA rates traumatic brain injuries based on the residual symptoms a veteran is currently experiencing because of the trauma under 38 CFR § 4.124a.
VA rates these residuals on a scale of 0, 1, 2, 3, or total, with each of these increments corresponding to a disability rating. Ratings range from 0 to 100 percent.
VA divides the rating criteria of TBI residuals into 10 subcategories in order to evaluate the condition. Veterans are then rated based on the level of severity and impairment in each of these areas of functioning:
- Impairment of memory, attention, concentration, and executive functions
- Altered judgement
- Inhibited social skills
- Orientation to person, time, place, and situation
- Impaired motor activity
- Visual-spatial orientation
- Subjective symptoms
- Neurobehavioral effects
- Ability to communicate
- Consciousness
TBI Presumptions
As of January 2014, VA presumes service connection for five diseases if precipitated by a service-connected TBI:
- Dementia
- Parkinson’s disease
- Seizures
- Depression
- Hormone deficiency
What Is PTSD?
VA presumes PTSD, or post-traumatic stress disorder, is a mental health condition that occurs as a result of experiencing a distressing, shocking, or otherwise traumatic event. Many veterans develop PTSD from events they witnessed or experienced during their military service.
Symptoms and severity of PTSD can vary from person to person, but the most common symptoms include:
- Re-experiencing the trauma through intrusive, distressing recollections of the event, flashbacks, and nightmares
- Emotional numbness and avoidance of places, people, and activities that are reminders of the trauma, as well as anxiety/depression
- Increased arousal such as difficulty sleeping and concentrating, feeling jumpy, and being easily irritated and angered
How Is PTSD Rated?
In order for VA to grant direct service connection for post-traumatic stress disorder, a veteran must provide proof of:
- A current diagnosis of PTSD;
- A statement from the veteran about the stressor that occurred during service; and
- A medical opinion that the stressor was sufficient to cause PTSD from a VA psychologist/psychiatrist, or a psychologist/psychiatrist under contract with VA
PTSD is then rated using the General Rating Formula for Mental Disorders. Ratings range from 0 to 100 percent, with intervals at 10, 30, 50, and 70 percent. Veterans do not need to experience each symptom listed in the criteria to be eligible for that rating.

100 percent–Total occupational and social impairment, due to such symptoms as:
- Gross impairment in thought processes or communication
- Persistent delusions or hallucinations
- Grossly inappropriate behavior
- Persistent danger of hurting self or others
- Intermittent inability to perform activities of daily living (including maintenance of minimal personal hygiene)
- Disorientation to time or place
- Memory loss for names of close relatives, own occupation, or own name
70 percent–Occupational and social impairment, with deficiencies in most areas, such as work, school, family relations, judgment, thinking, or mood, due to such symptoms as:
- Suicidal ideation
- Obsessional rituals which interfere with routine activities
- Speech intermittently illogical, obscure, or irrelevant
- Near-continuous panic or depression affecting the ability to function independently, appropriately, and effectively
- Impaired impulse control (such as unprovoked irritability with periods of violence)
- Spatial disorientation; neglect of personal appearance and hygiene
- Difficulty in adapting to stressful circumstances (including work or a work-like setting)
- Inability to establish and maintain effective relationships
50 percent–Occupational and social impairment with reduced reliability and productivity due to such symptoms as:
- Flattened affect
- Circumstantial, circumlocutory, or stereotyped speech
- Panic attacks more than once a week
- Difficulty in understanding complex commands
- Impairment of short- and long-term memory (e.g., retention of only highly learned material, forgetting to complete tasks)
- Impaired judgment
- Impaired abstract thinking
- Disturbances of motivation and mood
- Difficulty in establishing and maintaining effective work and social relationships
30 percent–Occupational and social impairment with occasional decrease in work efficiency and intermittent periods of inability to perform occupational tasks (although generally functioning satisfactorily, with routine behavior, self-care, and conversation normal), due to such symptoms as:
- Depressed mood
- Anxiety
- Suspiciousness
- Panic attacks (weekly or less often)
- Chronic sleep impairment
- Mild memory loss (such as forgetting names, directions, recent events)
10 percent–Occupational and social impairment due to mild or transient symptoms that decrease work efficiency and ability to perform occupational tasks only during periods of significant stress, or symptoms controlled by continuous medication.
0 percent–A mental condition has been formally diagnosed, but symptoms are not severe enough either to interfere with occupational and social functioning OR to require continuous medication.
Understanding the Connection Between TBI and PTSD
Overlapping Causes & Symptoms
Many of the symptoms associated with TBI overlap with common symptoms of PTSD, as well as those of other similar conditions. Due to this overlap, it can be challenging to determine the underlying issue.
For example, depression, trouble sleeping, and memory problems can occur in cases of TBI and with PTSD. Additionally, many veterans with TBIs also develop PTSD. Veterans who suffered TBIs during their military service are often more likely to develop PTSD.
Traumatic brain injuries often involve both physical and emotional trauma (e.g., fear from a near-death experience), and emotional trauma can be a stressor that causes a veteran to develop PTSD. Similarly, the stress of a TBI can worsen a veteran’s pre-existing mental health condition.

Will VA Rate TBI and PTSD Separately?
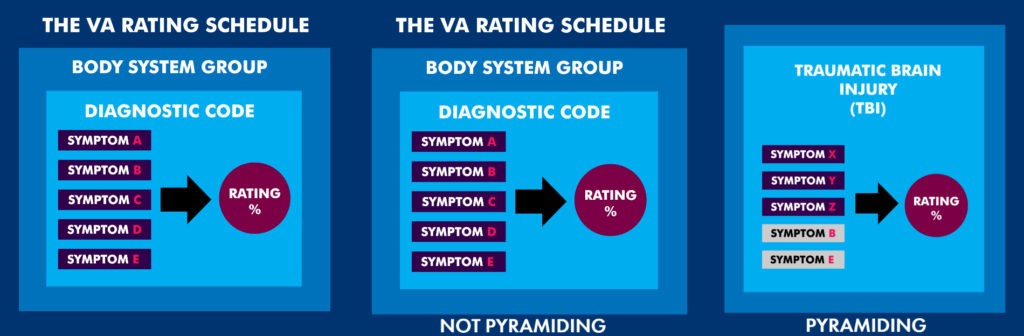
Since TBI and PTSD share certain symptoms, it is important to note that the same symptoms cannot be used to rate two separate disorders.
Pyramiding is the VA term for rating the same disability – or same manifestation (i.e., symptom) of a disability – twice.
For example, a veteran is service connected for PTSD due to an in-service combat event and experiences flashbacks, hypervigilance, social isolation, and has severe trouble falling and staying asleep (i.e., sleep impairment) and is highly irritable around others. Their PTSD rating takes those symptoms into account.
Later, it becomes clear that the veteran also suffered a TBI. Sleep impairment and irritability, in addition to being symptoms of PTSD, are core symptoms of traumatic brain injury.
If the veteran was being rated for just one of these conditions, sleep impairment and irritability would both be factored into a VA rater’s assessment of the veteran’s TBI or PTSD rating.
However, if the veteran is diagnosed with PTSD and TBI, certain symptoms/residuals (i.e., sleep impairment) can only be factored into the rating for one condition, not both.
In this example, VA might consider the veteran’s sleep impairment and irritability when rating the TBI but not the PTSD.
By law, VA must choose whichever condition would give the veteran the highest overall rating.
Special Monthly Compensation for TBI
Veterans who suffer debilitating residuals of a TBI may qualify for SMC(t), a level of special monthly compensation reserved specifically for veterans who have suffered traumatic brain injuries. Criteria for SMC(t) includes:
- The veteran needs regular Aid and Attendance for residuals of a TBI.
- The veteran is not eligible for a higher level of A&A under SMC (R)(2).
- The veteran would need hospitalization, nursing home care, or other residential institutional care without in-home A&A.
VA Compensation Amounts for PTSD and TBI
The amount of compensation a veteran can receive is the same at each rating level, no matter the condition.
Starting in December 2023, a 100 percent disability rating would equal $3,737.85 per month for PTSD or TBI, while a 50 percent disability rating would equal $1,075.16 per month.
However, veterans who are rated for multiple conditions, such as TBI and PTSD, will receive a combined disability rating that may result in increased compensation.
For example, a 30 percent PTSD rating and 10 percent TBI rating would be combined using VA math to equal a 37 percent combined rating, resulting in a 40 percent combined rating.
CCK’s VA Disability Calculator can be a great asset for help with VA math.
Getting Accredited Representation for TBI or PTSD Rating
If your claim for VA disability benefits for traumatic brain injury or post-traumatic stress disorder has been denied, help may be available to you. The experienced team of veterans’ advocates at Chisholm Chisholm & Kilpatrick has helped veterans diagnosed with both TBI and PTSD win the benefits they deserve.
Call our office today at 800-544-9144 for a free case evaluation to see if we may be able to assist.
About the Author
Share this Post
