Pyramiding: How to Avoid Stacking Your VA Ratings
CCK Law: Our Vital Role in Veterans Law
VA pyramiding is the prohibited practice of rating the same disability symptom more than once across different diagnostic codes. Under 38 CFR § 4.14, VA is forbidden from compensating veterans twice for the same symptom—even when that symptom stems from two separate service-connected conditions.
The rule sounds simple, but it is frequently misapplied. VA raters sometimes deny a legitimate separate rating by incorrectly calling it pyramiding, costing veterans compensation they are legally entitled to receive.
A few key points to understand before reading further:
- VA rates symptoms, not diagnoses. The pyramiding rule targets duplicate compensation for the same symptom, not the same condition.
- Separate ratings are allowed when two conditions produce truly distinct, non-overlapping symptoms.
- Mental health conditions are the most common pyramiding scenario for veterans—nearly all psychiatric diagnoses share a single rating formula under 38 CFR § 4.130.
- VA must assign overlapping symptoms to whichever diagnostic code benefits the veteran most.
Who We Are: Chisholm Chisholm & Kilpatrick (CCK Law) has argued many of the cases that have defined and clarified veterans disability law. CCK Law attorneys serve in leadership positions throughout the legal community and have posted more than 2,500 blogs and 1,100 videos about veterans benefits.

What Is VA Pyramiding?
Pyramiding is VA’s term for rating the same disability—or, more accurately, the same manifestation (symptom) of a disability—under more than one diagnostic code. 38 CFR § 4.14 prohibits this practice under the heading “Avoidance of Pyramiding,” stating that “the evaluation of the same disability under various diagnoses is to be avoided.”
The purpose of VA disability compensation is to compensate veterans for the average reduction in earning capacity caused by their service-connected conditions. As the U.S. Court of Appeals for Veterans Claims held in Brady v. Brown, 4 Vet. App. 206 (1993), the rating schedule “may not be employed as a vehicle for compensating a claimant twice (or more) for the same symptomatology; such a result would overcompensate the claimant for the actual impairment of his earning capacity.”
What Does “Same Disability” Actually Mean Under the Pyramiding Rule?
The text of 38 CFR § 4.14 refers to “the same disability,” but in practice, VA raters interpret this at the level of individual symptoms, or what VA often calls “residuals.”
A practical translation of the rule: “The evaluation of the same symptom under various diagnostic codes is to be avoided.”
This matters because two different diagnoses can produce some of the same symptoms. When they do, the question is not whether the veteran has two diagnoses; it is whether the rating for each diagnosis is counting the same symptom.
What Symptoms Does VA Associate With Each Disability?
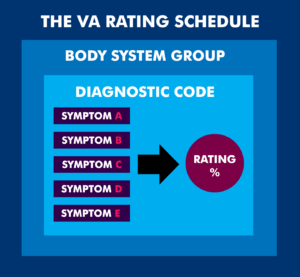
VA uses a detailed guide called the VA Schedule of Rating Disabilities (VASRD)—commonly called the VA Rating Schedule—to determine the symptoms (or residuals) and severity of each service-connected condition.
The Rating Schedule is organized by bodily system. Each system contains a list of conditions, each assigned a diagnostic code (DC). Under each diagnostic code, VA provides rating criteria: combinations of symptoms that correspond to specific disability percentages, typically in 10-percent increments.
Example: PTSD and TBI
A commonly cited example of pyramiding involves a veteran with both post-traumatic stress disorder (PTSD) and a traumatic brain injury (TBI), two conditions that frequently share symptoms.
Say VA has granted service connection for a veteran’s PTSD related to an in-service combat event. In addition to flashbacks, hypervigilance, and social isolation, the veteran experiences severe sleep impairment and significant irritability. Their PTSD rating reflects those symptoms.
It later becomes clear that the same combat event also caused a TBI. Sleep impairment and irritability are core symptoms of TBI as well. Even though these are separate conditions, a veteran’s rating may not change if there are no new or worsened symptoms.
What Would Make It Pyramiding?
If sleep impairment was factored into both the PTSD rating and the TBI rating, that would be pyramiding: the same symptom counted twice under two separate diagnostic codes.
The same would be true if irritability was also considered under both ratings. Any symptom counted twice, regardless of which two conditions share it, constitutes prohibited pyramiding under 38 CFR § 4.14.

What Would NOT Make It Pyramiding?
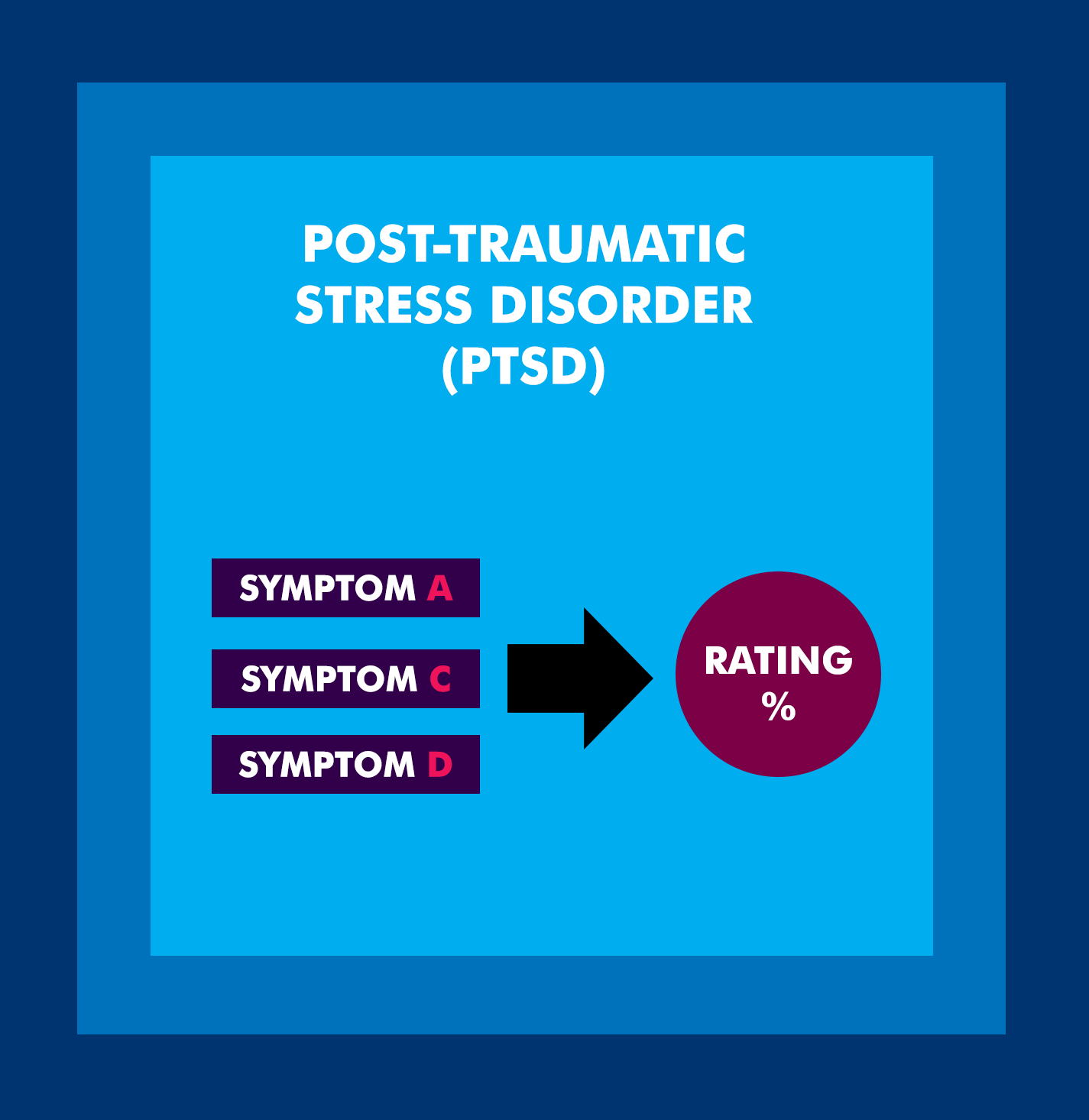
To avoid pyramiding, VA should factor the shared symptoms (sleep impairment, irritability) into the rating for one condition only, not both. Any symptoms unique to each condition are then rated separately under their respective diagnostic codes.
In the PTSD/TBI example: If sleep impairment and irritability are counted under the TBI rating, the PTSD rating should reflect only PTSD-exclusive symptoms such as flashbacks, hypervigilance, and avoidance behaviors.
This is how two separate ratings can coexist without violating the anti-pyramiding rule.
Which Diagnostic Code Gets the Overlapping Symptom?
When a symptom is shared across two conditions, 38 CFR § 4.7 requires VA to assign the higher of two evaluations when there is doubt as to the appropriate rating level, and VA’s overall duty to maximize benefits—grounded in 38 CFR § 3.102 and 38 CFR § 4.3—requires it to resolve reasonable doubt in the veteran’s favor.
In practice, VA should assign the overlapping symptom to whichever condition will yield the highest overall combined rating for the veteran. Assigning the symptom to a lower-rated condition when a higher-rated one is available would effectively undercompensate the veteran.
Does Pyramiding Apply to Mental Health Conditions?
Yes, and this is especially important for veterans with multiple psychiatric diagnoses.
VA rates nearly all mental health conditions—including PTSD, major depressive disorder, generalized anxiety disorder, bipolar disorder, and most others—under a single General Rating Formula for Mental Disorders at 38 CFR § 4.130. This formula rates all mental health conditions on the same scale of occupational and social impairment, with possible ratings of 0, 10, 30, 50, 70, or 100 percent.
Because essentially all mental health conditions are evaluated using the same criteria, VA will almost never assign separate ratings for co-occurring psychiatric diagnoses. A veteran with both PTSD and major depressive disorder, for example, will receive a single combined mental health rating, not separate ratings for each diagnosis.
This is consistent with VA’s own regulatory commentary acknowledging that mental disorders are “composed of multiple emotional, cognitive, and behavioral dimensions, many of which are shared across disorders,” and that comorbidity among mental health conditions “is the rule rather than the exception.”
What Does This Mean in Practice?
- PTSD + depression: One combined mental health rating. VA will not assign separate ratings for both.
- PTSD + anxiety: One combined mental health rating.
- Depression + anxiety: One combined mental health rating.
- PTSD + TBI (cognitive symptoms): Separate ratings may be possible if the TBI produces distinct cognitive or neurological symptoms—such as memory impairment or impaired executive function—that are genuinely separate from the psychiatric symptoms being rated under the mental health formula.
For more on how VA rates depression and anxiety together, see CCK’s guide on VA disability ratings for depression and anxiety.
Does Pyramiding Apply to Digestive Conditions Like IBS and GERD?
This area of VA law changed significantly in 2024.
Before May 19, 2024, VA’s rating schedule for digestive conditions generally prohibited separate ratings for conditions such as irritable bowel syndrome (IBS) and gastroesophageal reflux disease (GERD), because both fell within overlapping diagnostic code groupings in the 38 CFR § 4.114 series.
Effective May 19, 2024, VA updated its digestive system rating schedule. GERD now has its own diagnostic code (DC 7206) and IBS has a revised diagnostic code (DC 7319). Because these updated codes address different parts of the gastrointestinal tract—GERD primarily affects the esophagus and stomach; IBS primarily affects the intestines—veterans may now receive separate ratings for GERD and IBS, if their specific symptoms do not overlap under 38 CFR § 4.14.
Veterans who were rated for GERD with IBS under the old schedule should consider consulting with an experienced VA-accredited representative to determine whether updated, separate ratings would be more beneficial.
When Do Separate Ratings NOT Constitute Pyramiding?
The landmark CAVC decision Esteban v. Brown, 6 Vet. App. 259 (1994) established the governing principle: A veteran is entitled to separate disability ratings for distinct conditions arising from the same injury, as long as the symptomatology for each condition is not duplicative of or overlapping with the others.
In Esteban, a veteran sustained a facial injury in military service. VA initially assigned a single rating for the scarring. The Court held that the veteran was actually entitled to three separate ratings—one for cosmetic disfigurement, one for painful scarring, and one for facial muscle damage affecting his ability to chew—because each involved different functional impairment and none of the symptom criteria overlapped.
The practical rule from Esteban: If you can clearly identify distinct symptoms attributable to each condition—and medical evidence supports that each symptom belongs to a different diagnostic code—separate ratings do not violate the anti-pyramiding rule.
Common examples where VA has permitted separate ratings:
- Musculoskeletal conditions affecting different joints (e.g., service-connected knee instability and knee limited extension may each warrant a separate rating if the symptoms are distinguishable)
- A physical condition and a psychiatric condition with truly non-overlapping symptoms
- TBI cognitive symptoms and PTSD psychiatric symptoms, in some cases, when a qualified examiner can clinically differentiate the two
Does VA Ever Misapply the Pyramiding Rule?
Yes, and it is a common problem. VA raters, particularly less experienced ones, sometimes deny a legitimate separate rating by incorrectly invoking the pyramiding rule when the veteran’s symptoms are, in fact, distinct.
The rule goes both ways:
- Over-applying pyramiding means denying a separate rating for conditions that truly produce non-overlapping symptoms. This results in a lower combined rating and less compensation than the veteran is entitled to.
- Under-applying pyramiding means allowing two ratings that count the same symptom twice. This can result in a rating reduction if VA later catches the error.
If VA makes a mistake, veterans have the right to challenge that decision through VA’s three review options under the Veterans Appeals Improvement and Modernization Act (AMA): a Supplemental Claim, a Higher-Level Review, or an appeal to the Board of Veterans’ Appeals. These tracks have very different evidence requirements, timelines, etc. We strongly recommend that you consider discussing your options with a VA-accredited lawyer or advocate.
Frequently Asked Questions About VA Pyramiding
What is VA disability pyramiding?
Pyramiding is VA’s term for the prohibited practice of rating the same disability symptom more than once, even when that symptom is shared by two separate service-connected conditions. It is prohibited under 38 CFR § 4.14.
Can I receive separate ratings for PTSD and depression?
Generally, no. VA uses a single General Rating Formula for Mental Disorders under 38 CFR § 4.130 for nearly all psychiatric diagnoses. Because the same rating criteria apply to both conditions, rating them separately would almost always involve counting overlapping symptoms twice.
Can I receive separate ratings for PTSD and TBI?
In some cases, yes. If the TBI produces distinct symptoms—such as cognitive impairment or neurological deficits—that do not overlap with the psychiatric symptoms being rated under PTSD, separate ratings may be appropriate. This determination is highly fact specific.
Does VA always decide correctly which diagnostic code gets an overlapping symptom?
No. VA sometimes assigns a shared symptom to the lower-value diagnostic code, which reduces a veteran’s overall combined rating. VA should assign overlapping symptoms to the code that produces the greatest benefit for the veteran.
What happens if VA incorrectly says my claim involves pyramiding?
Veterans have the right to appeal. Under the AMA appeals system, options include a Supplemental Claim (with new and relevant evidence), a Higher-Level Review, or an appeal to the Board of Veterans’ Appeals. Medical evidence clearly attributing distinct symptoms to specific conditions is critical to a successful appeal.
Can I get separate ratings for GERD and IBS?
As of May 19, 2024, yes, in most cases. VA’s updated digestive rating schedule now assigns GERD and IBS to different diagnostic codes addressing different parts of the gastrointestinal tract. Separate ratings are permissible if symptoms do not overlap under 38 CFR § 4.14.
Is “rating stacking” the same as pyramiding?
Yes. Veterans and practitioners sometimes use “rating stacking” and “pyramiding” interchangeably. Both refer to the prohibited practice of counting the same symptom under more than one diagnostic code.
About the Author
Share this Post
