VA Secondary Conditions to GERD and VA Ratings

CCK Law: Our Vital Role in Veterans Law
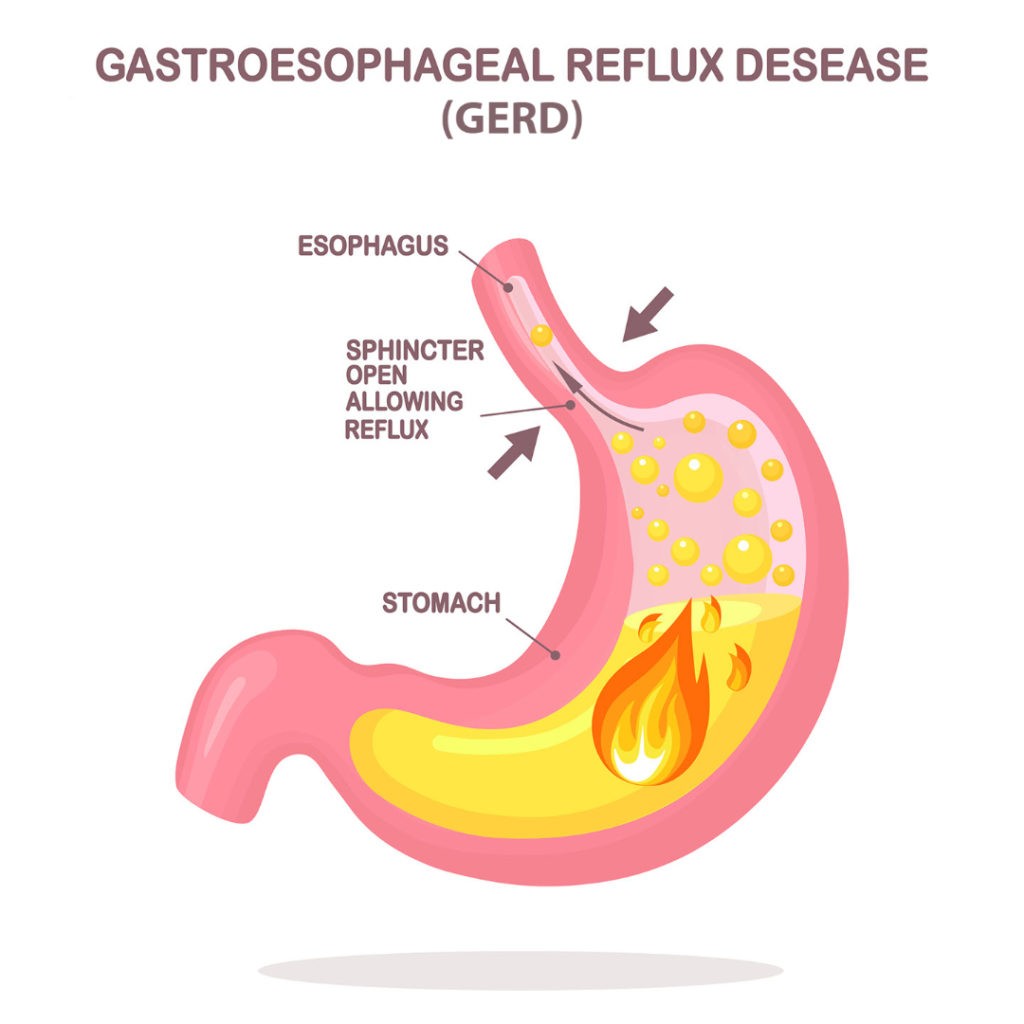
What is Gastroesophageal Reflux Disease (GERD)?
Gastroesophageal Reflux Disease, or GERD, is a chronic digestive condition characterized by stomach acid flowing back up the esophagus, causing discomfort and inflammation and may be a secondary condition to many disabilities.
A sphincter at the bottom of the esophagus that allows food to pass into your stomach usually prevents it from traveling back up. When the sphincter is weakened, stomach acid can travel back up the esophagus. This leads to heartburn and acid reflux, the two primary indicators of GERD.
Possible Symptoms of GERD
- Heartburn
- Nausea
- Vomiting
- Difficulty breathing
- Chronic coughing
- Chronic sore throat
- Painful swallowing
- Chest pain
- Cavities
- Inflammation of the gums
- Abdominal pain
Doctors generally recommend lifestyle changes (e.g., dietary changes, quitting smoking, or losing weight) or certain medications (e.g., antacids, proton pump inhibitors, or H2 blockers) to treat symptoms of gastroesophageal reflux disease. If symptoms do not improve with lifestyle changes or medication, surgery is sometimes recommended.
GERD Among Veterans
Many veterans experience heartburn and acid reflux following separation from active military service, perhaps brought on by an in-service occurrence. Veterans who have very frequent episodes of heartburn often develop GERD.
GERD may also occur due to another existing condition, such as a hernia, migraines, or chronic obstructive pulmonary disease (COPD). GERD is also linked to mental health conditions that are common among veterans, such as post-traumatic stress disorder (PTSD) and anxiety.
GERD Secondary to PTSD;
There are several possible reasons why PTSD may lead to a veteran developing GERD. Selective serotonin reuptake inhibitors (SSRIs), which veterans take to treat their PTSD symptoms, have side effects that cause digestive issues, like GERD. There is also medical evidence suggesting that PTSD can cause an overproduction of stomach acid, which may lead to GERD.
PTSD is rated using the General Rating Formula for Mental Disorders. Veterans can be rated at 0, 10, 30, 50, 70, or 100 percent.
GERD Secondary to Anxiety and Depression
Anxiety and depression, like PTSD, may worsen symptoms like acid reflux that lead to GERD.
According to VA, around 11 percent of veterans have reported elevated levels of depression and around 10 percent have reported elevated levels of anxiety. Studies also suggest that anxiety and depression levels are significantly higher in patients with gastroesophageal reflux disease.
Depression and anxiety are also rated using the General Rating Formula for Mental Disorders. Veterans can be rated at 0, 10, 30, 50, 70, or 100 percent.

VA Disability Ratings for GERD
The U.S. Department of Veterans Affairs rates GERD under 38 CFR § 4.114, Schedule of Ratings – Digestive System, Diagnostic Code 7206. Ratings are assigned based on severity of symptoms.
Veterans can be rated at 0, 10, 30, 50, or 80 percent, depending on the severity of their disability. The criteria for each VA rating are as follows:
• 80 percent – “Documented history of recurrent or refractory esophageal esophageal stricture(s) causing dysphagia with at least one of the symptoms present: (1) aspiration, (2) undernutrition, and/or (3) substantial weight loss as defined by § 4.112(a) and treatment with either surgical correction or percutaneous esophagogastrointestinal tube (PEG tube)”
• 50 percent – “Documented history of recurrent or refractory esophageal stricture(s) causing dysphagia which requires at least one of the following (1) dilatation 3 or more times per year, (2) dilatation using steroids at least one time per year, or (3) esophageal stent placement”
• 30 percent – “Documented history of recurrent esophageal stricture(s) causing dysphagia which requires dilatation no more than 2 times per year”
• 10 percent – “Documented history of esophageal stricture(s) that requires daily medications to control dysphagia otherwise asymptomatic”
• 0 percent – “Documented history without daily symptoms or requirement for daily medications”
What is a Secondary VA Disability?
A secondary condition is a disability or disease that develops as the result of a service-connected condition. Secondary service connection is granted when a veteran proves a nexus, or link, between the secondary condition and the primary service-connected condition.
To secure secondary service connection and additional VA compensation, veterans must provide evidence of the following two things:
- A diagnosis for the secondary condition by a medical professional; and
- A medical opinion, or nexus, linking the secondary disability to the already service-connected condition.
Veterans will receive the same amount of VA compensation for a condition whether it is service-connected on a secondary or direct basis.
Sleep Apnea Secondary to GERD
Sleep apnea is a serious sleep disorder in which a person’s breathing is repeatedly interrupted throughout the night. Studies indicate that GERD can cause or aggravate sleep apnea, just as sleep apnea can cause or aggravate GERD.
There are three types of sleep apnea:
- Obstructive: the most common form of sleep apnea; occurs when the throat muscles intermittently relax and block airways during sleep.
- Central: occurs when the brain does not send the right signals to the muscles that control breathing.
- Complex (Mixed): occurs when someone has both obstructive and central sleep apnea.
VA rates sleep apnea at 0, 30, 50, or 100 percent, depending on the severity.
Asthma Secondary to GERD
Asthma is a respiratory condition in which a person’s airways become inflamed and narrow, making it difficult to breathe. Symptoms include coughing, wheezing, or shortness of breath.
Veterans with GERD may suffer from chest distress and symptoms of asthma. If someone already diagnosed with asthma develops GERD, the condition may worsen or trigger asthma symptoms.
VA rates asthma under 38 CFR § 4.97, Diagnostic Code 6602, ranging from 0 to 100 percent. A 100 percent rating is assigned to veterans who experience more than one asthma attack a week with episodes of respiratory failure, and who require daily use of systemic high dose corticosteroids or immunosuppressive medications.
Sinusitis Secondary to GERD
Chronic sinusitis occurs when the spaces inside your nose and head (i.e., sinuses) are swollen and inflamed for three months or longer, despite treatment. GERD may increase the risk of chronic sinusitis in adults, as stomach acid can travel up and inflame the nose and sinuses.
Sinusitis usually leads to a stuffy nose which makes breathing through the nose difficult. Other common symptoms include swollen eyes, ear pain, reduced sense of smell and taste, coughing or throat clearing, fatigue, and more.
Service-connected chronic sinusitis can be rated at 0, 10, 30, or 50 percent depending on how incapacitating it is for the veteran.

Did VA Deny Your Disability Claim?
If your claim for benefits to a condition secondary to GERD was denied, an experienced veterans’ advocate at Chisholm Chisholm & Kilpatrick LTD may be able to help. Appealing a VA decision can be long and difficult to navigate, and CCK can help ease the process.
Contact CCK today for a free case evaluation at 800-544-9144.
About the Author
Share this Post