VA Disability Benefits for Hypertension Secondary to PTSD

CCK Law: Our Vital Role in Veterans Law
What Is Hypertension?
Hypertension is a term used to describe high blood pressure. Blood pressure is determined both by the amount of blood your heart pumps and the amount of resistance to blood flow in your arteries. The more blood your heart pumps and the narrower your arteries, the higher your blood pressure.
Hypertension can lead to severe health complications and increase the risk of heart disease, stroke, and sometimes death.
Blood pressure is measured using two numbers:
- Systolic blood pressure–Measures the pressure in your arteries when your heart beats
- Diastolic blood pressure–Measures the pressure in your arteries when your heart rests between beats
Generally speaking, a normal blood pressure level is less than 120 systolic and 80 diastolic. If a person’s blood pressure is not within this range, they are considered to have hypertension.
What Is PTSD?
Post-traumatic stress disorder (PTSD) is a mental health condition that can develop in a person who has experienced or witnessed a distressing, shocking, or otherwise traumatic event.
Unfortunately, many veterans experience PTSD stemming from their military service. The symptoms of PTSD can often be very debilitating and have a negative impact on an individual’s daily life.
Symptoms of PTSD can include:
- Intrusive thoughts
- Avoidance
- Overwhelmingly negative thoughts and feelings
- Arousal and reactive symptoms
What Is VA Secondary Service Connection?
A secondary service-connected condition is one that results from or is aggravated by an already service-connected condition. In the case of hypertension and PTSD, hypertension would be the secondary condition that is caused or aggravated by the PTSD.
Filing a claim for secondary service connection is much like filing a regular claim for direct service connection. Veterans may submit a claim for secondary service connection on VA Form 21-526EZ, the same form they would use to file a regular claim.
When filing a claim for secondary service connection, veterans will need to demonstrate:
- A diagnosis for the secondary condition; and
- Medical evidence indicating the link between the primary service-connected condition and the secondary condition.

Prevalence of PTSD Among Veterans
PTSD is a very common condition among veterans. According to VA, the number of veterans with PTSD varies by service era:
- Operations Iraqi Freedom (OIF) and Enduring Freedom (OEF)–About 11–20 out of every 100 veterans (i.e., between 11 and 20 percent) who served in OIF or OEF have PTSD in a given year.
- Gulf War (Desert Storm)–About 12 out of every 100 Gulf War veterans (12 percent) have PTSD each year.
- Vietnam War–About 15 out of every 100 Vietnam veterans (15 percent) were diagnosed with PTSD at the time of the most recent study in the late 1980s, the National Vietnam Veterans Readjustment Study (NVVRS). It is estimated that about 30 out of every 100 (30 percent) Vietnam veterans have had PTSD in their lifetime.
However, these statistics may not reflect the true number of veterans affected by PTSD, since not every veteran receives treatment for their PTSD-related symptoms.
VA’s 2020 Annual Benefits Report found that PTSD was the eighth most prevalent condition among new compensation recipients. Essentially, this means that PTSD is one of the more common conditions for newly service-connected veterans.
The 2020 report also noted that PTSD was the fourth most common service-connected disability among all veterans receiving disability benefits. Approximately 1.1 million veterans are service-connected for PTSD, as of 2020.
It is the most common mental health disability among service-connected veterans. Major depressive disorder and chronic adjustment disorder were the next most common mental health disabilities.
What Causes PTSD Among Veterans?
PTSD can be caused by a traumatic event, which is commonly referred to as a “stressor.” Veterans may have more than one stressor that impacts their PTSD.
Some stressors may include exposure to danger, such as death or injury, threats of danger, sexual trauma, or threats of sexual trauma. Veterans can also be exposed to trauma through witnessing it, or they may be indirectly exposed if someone they care about experiences trauma.
Examples of PTSD Stressors for Veterans
- Experiencing an IED explosion
- Witnessing a fellow service member be injured or killed
- Witnessing the death or injury of a civilian
- Being part of a burial crew
- Experiencing injury as a result of combat
- Being assaulted
- Being threatened with assault
- Military sexual trauma
- Threats of military sexual trauma

Can PTSD Cause Hypertension?
Studies have indicated there is a link between hypertension and PTSD. Specifically, in a group of nearly 200,000 veterans who served between September 2001 and July 2010, a diagnosis of PTSD left untreated was associated with a 24–46 percent greater risk of hypertension. The findings of this specific study were consistent among male and female veterans.
The connection between PTSD and hypertension may be due to several different factors. One of the most likely is that PTSD often causes physiological symptoms. These symptoms can include:
- Recurrent, involuntary, or intrusive and distressing memories of trauma
- Recurrent distressing dreams related to trauma
- Flashbacks or dissociative events where the veteran may feel as though the trauma is recurring
- Intense or prolonged psychological distress due to exposure to anything that resembles the trauma
- Physiological reactions to anything that reminds the veteran of the trauma
- Irritable or aggressive behavior
- Reckless or self-destructive behavior
- Hypervigilance
- Exaggerated startle response
- Difficulty concentrating
- Insomnia
As the body tends to undergo changes in arousal, reactivity, and heightened sensitivity with PTSD (e.g., fight or flight mode), the body may also experience persistent, prolonged high stress. The high level of stress that accompanies PTSD may cause veterans to experience hypertension.
How Does VA Rate PTSD?
PTSD is rated as a mental health disability under 38 CFR § 4.130. Ratings range from 0, 10, 30, 50, 70, and 100 percent based on:
- The level of social and occupational impairment; and
- The frequency, duration, and severity of the symptoms listed in the criteria.
However, the symptoms listed are not exhaustive. They are meant to serve as a guide for the level of impairment at each rating.
100 percent–Total occupational and social impairment, due to such symptoms as:
- Gross impairment in thought processes or communication
- Persistent delusions or hallucinations
- Grossly inappropriate behavior
- Persistent danger of hurting self or others
- Intermittent inability to perform activities of daily living (including maintenance of minimal personal hygiene)
- Disorientation to time or place
- Memory loss for names of close relatives, own occupation, or own name
70 percent–Occupational and social impairment, with deficiencies in most areas, such as work, school, family relations, judgment, thinking, or mood, due to such symptoms as:
- Suicidal ideation
- Obsessional rituals that interfere with routine activities
- Speech intermittently illogical, obscure, or irrelevant
- Near-continuous panic or depression affecting the ability to function independently, appropriately, and effectively
- Impaired impulse control (such as unprovoked irritability with periods of violence)
- Spatial disorientation
- Neglect of personal appearance and hygiene
- Difficulty in adapting to stressful circumstances (including work or a work-like setting)
- Inability to establish and maintain effective relationships
50 percent–Occupational and social impairment with reduced reliability and productivity due to such symptoms as:
- Flattened affect
- Circumstantial, circumlocutory, or stereotyped speech
- Panic attacks more than once a week
- Difficulty in understanding complex commands
- Impairment of short- and long-term memory (e.g., retention of only highly learned material, forgetting to complete tasks)
- Impaired judgment
- Impaired abstract thinking
- Disturbances of motivation and mood
- Difficulty in establishing and maintaining effective work and social relationships
30 percent–Occupational and social impairment with occasional decrease in work efficiency and intermittent periods of inability to perform occupational tasks (although generally functioning satisfactorily, with routine behavior, self-care, and conversation normal), due to such symptoms as:
- Depressed mood
- Anxiety
- Suspiciousness
- Panic attacks (weekly or less often)
- Chronic sleep impairment
- Mild memory loss (such as forgetting names, directions, recent events)
10 percent–Occupational and social impairment due to mild or transient symptoms that decrease work efficiency and ability to perform occupational tasks only during periods of significant stress, or symptoms controlled by continuous medication.
0 percent–A mental condition has been formally diagnosed, but symptoms are not severe enough either to interfere with occupational and social functioning OR to require continuous medication.
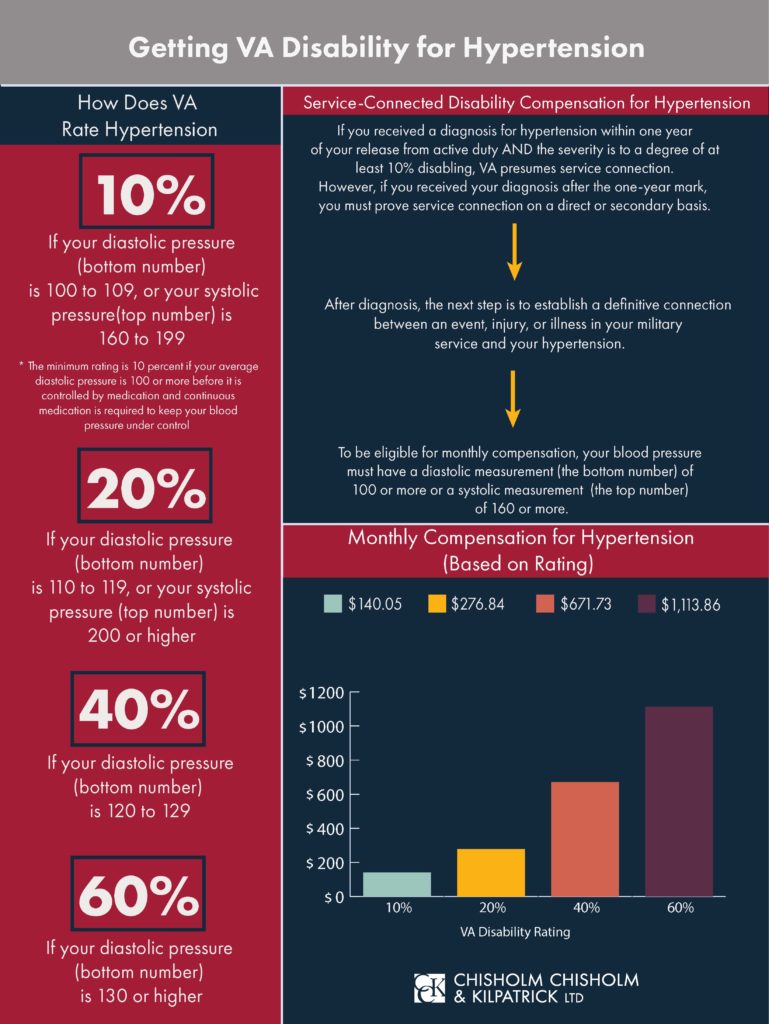
How Does VA Rate Hypertension?
VA uses 38 CFR § 4.104 – Schedule of Ratings, Cardiovascular System, Diagnostic Code 7101 to rate hypertension. VA rates hypertension the same whether service connection is established directly, presumptively, or secondarily due to PTSD.
The rating criteria are as follows:
- 60 percent–Diastolic pressure predominantly 130 or more
- 40 percent–Diastolic pressure predominantly 120 or more
- 20 percent–Diastolic pressure predominantly 110 or more, or; systolic pressure predominantly 200 or more
- 10 percent–Diastolic pressure predominantly 100 or more, or; systolic pressure predominantly 160 or more, or; minimum evaluation for an individual with a history of diastolic pressure predominantly 100 or more who requires continuous medication for control
Achieving TDIU Requirements With Hypertension Secondary to PTSD
Total disability based on individual unemployability, or TDIU, is a monthly benefit available to veterans who are prevented from working or maintaining employment because of their service-connected disabilities. TDIU pays veterans at the 100 percent rating level, even if their combined rating does not meet 100 percent.
VA outlines TDIU regulations under 38 CFR § 4.16, which includes subsections (a) and (b). To qualify for TDIU under 38 CFR § 4.16(a), or schedular TDIU, a veteran must have:
- One service-connected condition rated at 60 percent or higher; or
- Two or more service-connected conditions, one of which is rated at 40 percent or higher, with a combined rating of 70 percent or higher.
With hypertension secondary to PTSD, the ratings for both PTSD and hypertension can contribute to the veteran’s overall combined rating and help a veteran meet the requirements for schedular TDIU.
For example, if a veteran has a rating of 50 percent for PTSD and a rating for hypertension secondary to PTSD at 30 percent, they would then be eligible for TDIU.
Veterans who do not meet the schedular requirements under 38 CFR § 4.16(a) may still be considered for extraschedular TDIU under § 4.16(b). If veterans do not meet the criteria for schedular TDIU, VA will determine if their case should be referred to the Director of Compensation Service for extraschedular consideration.
Getting Accredited Representation for Hypertension Secondary to PTSD
If your claim for hypertension secondary to PTSD, or service connection for PTSD, was denied, you may want an accredited representative to assist with your appeal. Accredited representatives can help answer questions veterans may have regarding the appeals process, as well as submit documentation such as evidence and arguments on behalf of the veteran.
If you need help pursuing your VA disability benefits, the accredited representatives at Chisholm Chisholm & Kilpatrick may be able to help. Call our office today for a free case evaluation.
About the Author
Share this Post