VA Disability Benefits for GERD

CCK Law: Our Vital Role in Veterans Law
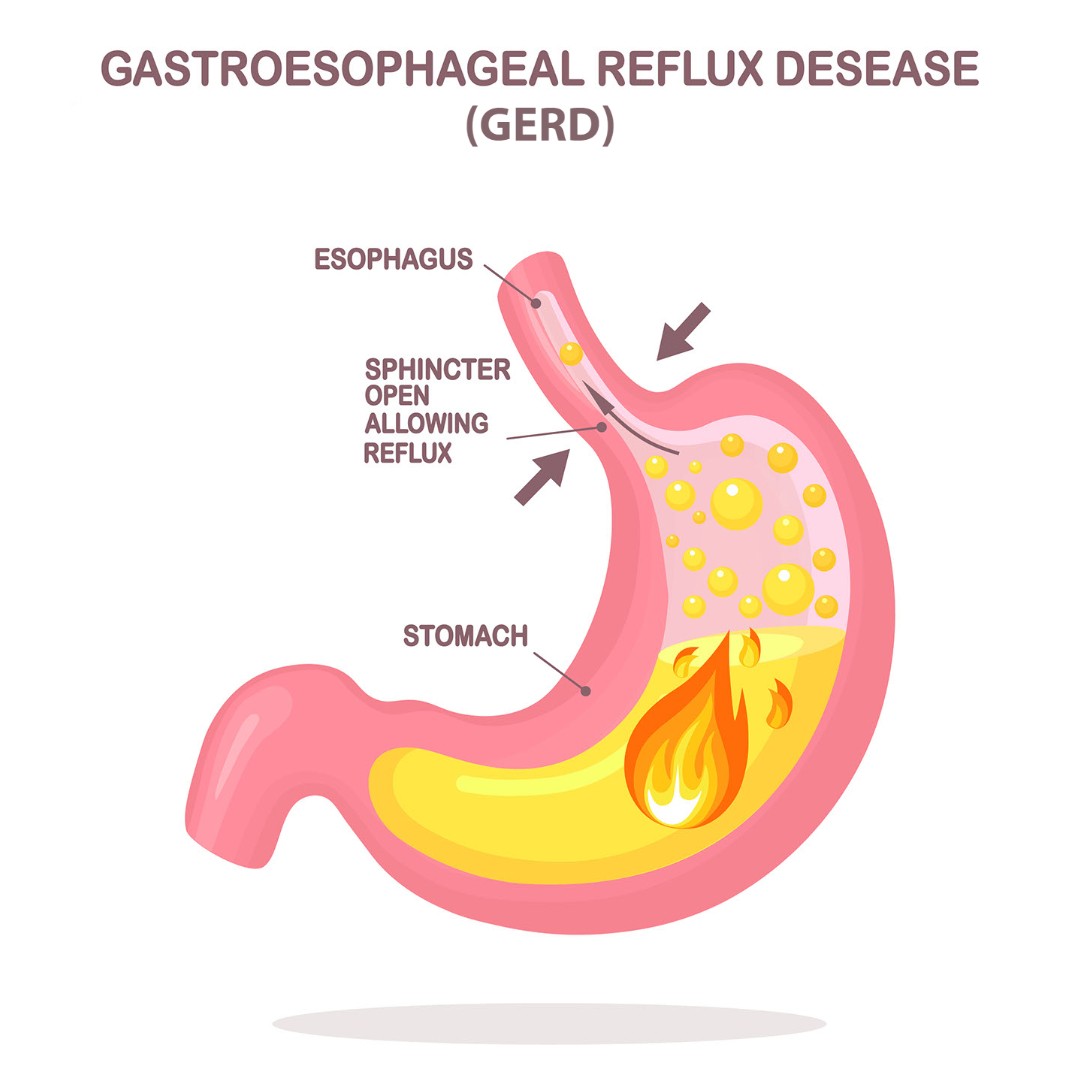
Gastroesophageal Reflux Disease (GERD) is a digestive disorder characterized by the occurrence of stomach acid flowing back up the esophagus from the stomach, causing discomfort and inflammation. GERD can typically be managed through lifestyle changes and diet, however, some may need medication to control their condition.
GERD is caused by frequent episodes of acid reflux. At the bottom of the esophagus, there is a sphincter that allows food to pass down into your stomach, and also prevents it from traveling back up your esophagus. When this sphincter is weak, stomach acid can travel up your esophagus. Common symptoms can include heartburn, difficulty swallowing, regurgitation, and chest pain.
Symptoms of GERD:
- Nausea
- Vomiting
- Heartburn
- Difficulty breathing
- Coughing
- Painful swallowing
- Chest pain
- Stomachaches or other abdominal pain
Risk Factors for GERD:
There are several risk factors that can cause GERD or exacerbate GERD for those who already experience it, including:
- Eating Certain Foods, specifically heavy meals immediately before lying down.
- Certain Medications, which can irritate the lining of the esophagus. These medications can include antibiotics, pain relievers, and iron pills.
- Smoking, which can increase acid secretion, reduce salivation, and damage muscles in the esophagus.
- Consumption of Alcohol, which may, in high amounts, weaken the muscles of the esophagus.
- Respiratory Conditions, such as COPD, can cause excessive coughing which can put a person at risk for developing GERD.
- Pregnancy, which can put pressure on the stomach and cause acid reflux.
- Obesity
Getting Service Connection for GERD
Most veterans will be service-connected for their GERD on a direct basis. Direct service connection requires three elements:
- A current diagnosis
- An in-service event, injury, or symptom
- A medical “nexus” linking the current diagnosis to the in-service occurrence.
There is no presumptive regulation that includes GERD. For example, GERD is not eligible for presumptive service connection as due to Agent Orange exposure or exposure to environmental hazards in the Persian Gulf War. Presumptive service connection is when VA presumes that a veteran’s current disability was caused by their time in service based on specific requirements such as the time period and location of the veteran’s service.
VA’s Persian Gulf War presumption regulation does allow for presumptive service connection for functional gastrointestinal disorders such as irritable bowel syndrome (IBS), functional constipation, functional vomiting, and functional dyspepsia. However, GERD is not considered to be a functional gastrointestinal disorder.
According to the International Foundation for Functional Gastrointestinal Disorders, “functional GI disorders are disorders of gut-brain interaction,” of which GERD is not considered to be.
Compensation and Pension (C&P) Exams for GERD
Compensation and Pension examinations are medical exams that VA requests to examine a veteran’s conditions or disabilities, in this case GERD. The exam will be performed by a VA physician or a VA-contracted physician. In GERD exams, the examiner may administer a blood test. This blood test can be used to screen for anemia.
The examiner may ask the veteran questions regarding their condition, their military service, or the link between their condition and service. The examiner may also examine the veteran to gather evidence regarding the connection between the veteran’s condition and their service. VA will use the evidence and information collected in this exam to help adjudicate the veteran’s claim.
C&P exams usually have a dual purpose:
- To confirm or deny service connection for the veteran’s claim; and
- To assess the severity of the claimed condition so that a rating may be issued in the event that service connection is confirmed.
The exam can last for a varying amount of time. Some exams may take only a few minutes while others may take several hours. Prior to the exam, the examiner should review the veteran’s entire claims file. The claims file includes all the previously submitted documentation, including evidence and medical treatment records. In most cases, the claims file also contains the veteran’s service records.
VA has a “duty to assist” in acquiring all the relevant evidence to the veteran’s claim. This means that VA should make all reasonable efforts to obtain evidence that supports the veteran’s claim. This evidence could include medical evidence which is crucial to the veteran’s disability case, such as records from a private physician.
In GERD cases, the veteran may want to consider using a Disability Benefits Questionnaire (DBQ). These forms are intended to quicken the time it takes to process claims and can help give veterans more control over the claims process. DBQs give veterans a space to answer questions about their disability relating to symptoms, severity, causes, and the relationship to other disabilities.
DBQs may also be filled out by a veteran’s treating physician or primary care doctor prior to the exam, giving the doctor who may be most knowledgeable about the veteran’s GERD the opportunity to provide input.
Tips for C&P Exams
Attendance – Veterans should be sure to attend C&P exams when VA schedules them. If a veteran does not attend a C&P exam, VA may deny their claim. Skipping an exam, especially without alerting VA, can be very detrimental to a veteran’s claim. VA will usually reach out to the veteran to schedule an exam via a phone call or a letter. If a veteran cannot attend an exam after it has been scheduled, the veteran should be sure to contact VA to reschedule. The veteran should also be sure to contact VA as soon as possible if they find out they have missed an exam.
Honesty – Oftentimes, veterans will downplay the severity of their conditions in a way that can be detrimental to their claim. It is important to be honest and thorough when speaking about the claimed condition. The examiner should give the opportunity for the veteran to speak about how their GERD impacts them, whether that be in severity or how it inhibits their day-to-day life. Including as much information as possible, while still being honest, can help to make sure that everything is considered when the claim is being adjudicated.
Persistence – After a C&P exam, VA does not usually give copies of the exam report to the veteran. Veterans will want to be sure to specifically request a copy of the exam to ensure they receive one. After receiving the copy, veterans should review to see if the report contains anything with which they disagree. Veterans may let VA know that they disagree with the report if they wish. They may also obtain an expert opinion of their own to refute the exam’s findings.
VA Disability Ratings for GERD Explained
Disability benefits are assigned in accordance with VA’s rating system. Ratings are assigned based on severity of symptoms, with the most severe conditions receiving the highest rating.
GERD is rated under 38 CFR § 4.114, Schedule of Ratings – Digestive System, Diagnostic Code 7206. Veterans can be rated at 0, 10, 30, 50, or 80 percent, depending on the severity of their disability. The criteria for each VA rating are as follows:
• 80 percent – “Documented history of recurrent or refractory esophageal esophageal stricture(s) causing dysphagia with at least one of the symptoms present:
- aspiration
- undernutrition, and/or
- substantial weight loss as defined by § 4.112(a) and treatment with either surgical correction or percutaneous esophagogastrointestinal tube (PEG tube)”
• 50 percent – “Documented history of recurrent or refractory esophageal stricture(s) causing dysphagia which requires at least one of the following:
- dilatation 3 or more times per year, or
- dilatation using steroids at least one time per year, or
- esophageal stent placement”’
• 30 percent – “Documented history of recurrent esophageal stricture(s) causing dysphagia which requires dilatation no more than 2 times per year”
• 10 percent – “Documented history of esophageal stricture(s) that requires daily medications to control dysphagia otherwise asymptomatic”
• 0 percent – “Documented history without daily symptoms or requirement for daily medications”
How to Increase Your VA Rating for GERD
In addition to the criteria listed above, if a veteran’s service-connected conditions prevent them from working, they may qualify to be compensated at the 100% rate through total disability based on individual unemployability (TDIU), even if their disabilities do not combine to a scheduler 100% through VA math.
Veterans may also be able to receive an increased rating, or more disability benefits, for GERD through secondary service connection. Secondary service connection refers to when a veteran is already service-connected for one condition which then causes or aggravates a second condition. This condition may not be directly related to service. The condition that is not connected directly to service, or rather the secondary condition, can then be granted service condition.
In order to establish secondary service connection, the veteran will need to demonstrate the link, or nexus, between the two conditions.
Common Conditions GERD May Be Secondary to:
- Post-Traumatic Stress Disorder, or PTSD—Veterans who were diagnosed with PTSD caused by their service may use SSRI medication, or selective serotonin reuptake inhibitors, to treat their symptoms. SSRI medication, however, can be linked to causing side effects such as GERD. As such, veterans can receive a VA rating for GERD as secondary to PTSD.
- Chronic Obstructive Pulmonary Disease, or COPD—Chronic coughing caused by COPD may irritate the esophagus which, in turn, could cause the veteran to develop GERD.
- Sleep Apnea—Veterans who suffer from sleep apnea may find that the condition aggravates or causes GERD. Specifically, while asleep the body may not clear the veteran’s esophagus as it would when the veteran is awake. This can exacerbate GERD. Additionally, GERD may contribute to sleep apnea, as acid in the esophagus can cause spasms in the vocal cords which may prompt sleep apnea.
- Migraines—Studies have also linked migraines and GERD. More specifically, those who experience migraines may find that the reflux symptoms of GERD are increased. Migraines may cause hypersensitivity to gastric distention, or the enlargement of the stomach. Those who experience service-connected migraines may be able to receive an additional VA disability rating for GERD through secondary service connection.
This list is certainly not exhaustive and there may be more pathways to allow GERD to become service-connected on a secondary basis.
Has your VA disability benefits claim for GERD been denied? Contact Chisholm Chisholm & Kilpatrick today
The appeals process at the Department of Veterans Affairs is often long and difficult to navigate. Although you are free to appeal unfavorable VA decisions on your own, an experienced VA-accredited attorney can help. The skilled attorneys at Chisholm Chisholm & Kilpatrick LTD has helped many veterans win the VA disability benefits to which they are entitled. Contact our office today for a free consultation at (800) 544-9144.
About the Author
Share this Post