VA Benefits for Dependents of Disabled Veterans

CCK Law: Our Vital Role in Veterans Law
What Are Dependents for VA Purposes?
For VA purposes, a dependent is a family member who relies on the veteran financially and meets certain criteria. Examples of dependents for VA purposes include:
- A spouse
- Unmarried children, including stepchildren, adopted children, and biological children, who:
- Are under the age of 18; or
- Are between the ages of 18 and 23 and attending school full-time; or
- Were seriously disabled prior to reaching age 18.
- Parents whose net worth and income are below the limit put in place by law
- Parents (biological, step, adopted, foster, etc.) are defined as those who, for at least one year, “stood in the relationship of a parent to a veteran at any time before their entry into active service.”
As a dependent of a veteran or service member, you may be eligible for certain benefits, such as health care, life insurance, or monetary compensation to help pay for school or vocational training. However, to qualify for many of these benefits, your veteran will likely have to have a combined disability rating of 30 percent or higher from VA.
Can I Gain Additional Compensation by Adding Dependents to a VA Claim?
Yes, veterans with a combined disability rating of 30 percent or higher can receive additional monthly compensation when they add dependents to their VA claim.
Check out the infographic below to see firsthand how much extra compensation spouses, children, and dependent parents can add to a claim:
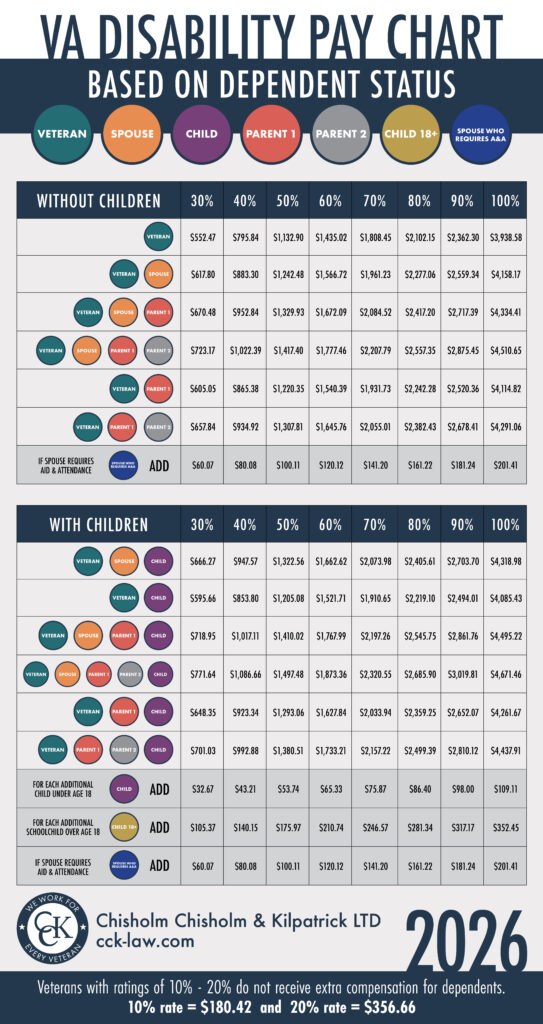
What Forms Should I Submit to Add Dependents to a VA Claim?
VA Form 21-686c is the form typically used to declare dependents and add them to a VA claim. However, there are situations where other forms might come in handy, including the following:
- Dependent parents can be added to a claim using VA Form 21P-509.
- Children between 18 and 23 who are enrolled in school can be added to a claim using VA Form 21-674.
- If the status of a dependent changes, veterans can update that status using VA Form 21-0538.
What Are VA Health Care Benefits for Dependents?
There are several health care options you may qualify for as the dependent of a veteran, including the following:
TRICARE
If you are a family member of an active duty, retired, or deceased service member, National Guard soldier, Reservist, or Medal of Honor recipient, you may qualify for the TRICARE program.
According to VA, TRICARE provides comprehensive health coverage, including health plans, prescription medicines, dental plans, and programs for people with special needs. This health care program is managed by the Department of Defense’s Defense Health Agency.
Civilian Health and Medical Program of the Department of Veterans Affairs (CHAMPVA)
The Civilian Health and Medical Program of the Department of Veterans Affairs (CHAMPVA) is a health benefits program in which VA shares the cost of certain health care services and supplies with eligible beneficiaries.
CHAMPVA is currently managed by the Veterans Health Administration Office of Community Care (VHA OCC) located in Denver, Colorado. The VHA OCC thereby processes all claims submitted for the reimbursement of medical services and supplies rendered by authorized providers in the community.
To be eligible, the beneficiary (i.e., person receiving the benefits) cannot be eligible for TRICARE. Importantly, TRICARE is the Department of Defense (DoD) health care program for uniformed service members, retirees, and their families. It provides comprehensive coverage to all beneficiaries, including health plans, special programs, prescriptions, and dental plans.
CHAMPVA is a completely separate program with a totally different beneficiary population than TRICARE. While the benefits are similar, the programs are administered separately with differences in claim filing procedures and preauthorization requirements. This program provides coverage to the spouse or widow and to the children of veterans who:
- Are rated permanently and totally disabled due to a service-connected condition; or
- Were rated permanently and totally disabled due to a service-connected condition at the time of death; or
- Died of a service-connected condition; or
- Died on active duty, and the dependents are not otherwise eligible for DoD’s TRICARE benefits.
As of October 1, 2001, these benefits were extended to individuals ages 65 and older. According to VA, this age group must meet the following conditions to be eligible:
- If the beneficiary was 65 or older prior to June 5, 2001, and was otherwise eligible for CHAMPVA, and was entitled to Medicare Part A coverage, then the beneficiary will be eligible for CHAMPVA without also requiring Medicare Part B coverage.
- If the beneficiary turned 65 before June 5, 2001, and has Medicare Parts A and B, the beneficiary must keep both Medicare Parts A and B to be eligible.
- If the beneficiary turned age 65 or older on or after June 5, 2001, the beneficiary must be enrolled in Medicare Parts A and B to be eligible.
Camp Lejeune Family Member Program
Veterans who served at Camp Lejeune for at least 30 cumulative days from August 1953 through December 1987, and their family members, may be eligible for health care benefits. Specifically, VA must reimburse dependents for out-of-pocket health care costs that were related to any of these 15 conditions:
- Bladder cancer
- Breast cancer
- Esophageal cancer
- Female infertility
- Hepatic steatosis
- Kidney cancer
- Leukemia
- Lung cancer
- Miscarriage
- Multiple myeloma
- Myelodysplastic syndromes
- Neurobehavioral effects
- Non-Hodgkin’s lymphoma
- Renal toxicity
- Scleroderma
To receive reimbursement for costs incurred during the treatment of a qualified condition listed above, you must first apply to the Camp Lejeune Family Member Program by completing VA Form 10-10068: Camp Lejeune Family Member Program Application and submitting it to VA, or you can do so online.
VA will require you to submit evidence proving your eligibility for the program, such as:
- Marriage license or birth certificate that shows a dependent relationship to a veteran who was stationed at Camp Lejeune
- Proof that you lived at the base for at least 30 days between August 1, 1953, and December 31, 1987. Such proof can include base housing records, military orders, utility bills, or tax forms.
- Medical records proving that you paid medical expenses for one of the qualifying conditions above, “respective to the following date ranges:”
- Dependents who lived at Camp Lejeune between January 1, 1957, and December 31, 1987, can be reimbursed for out-of-pocket medical expenses incurred on or after August 6, 2012.
- Dependents living at Camp Lejeune between August 1, 1953, and December 31, 1956, can have medical expenses incurred due to a qualifying condition reimbursed for care received on or after December 16, 2014.
- VA Form 10-10068b: Camp Lejeune Family Member Program Treating Physician Report completed by your doctor.
Spina Bifida Health Care Benefits Program
VA provides monetary allowances, vocational training, and rehabilitation and VA-financed health care benefits to certain Korea and Vietnam veterans’ birth children who have been diagnosed with spina bifida.
For the purposes of the VA Spina Bifida Health Care Program, spina bifida is defined as all forms or manifestations of spina bifida, except spina bifida occulta.
Children of Women Vietnam Veterans Health Care Benefits Program
VA also provides VA-financed health care benefits to women Vietnam veterans’ birth children who the Veterans Benefits Administration (VBA) has determined have a covered birth defect.
This program is not a comprehensive health care plan and only covers those services necessary for the treatment of a covered birth defect and associated medical conditions. It does not cover care that is unrelated to a covered birth defect.
Children whose biological mother is a Vietnam veteran and who were conceived after the date the veteran entered the Republic of Vietnam (period beginning February 28, 1961, and ending May 7, 1975), and who have one of the covered birth defects as determined by VBA are eligible for the program.
Pharmacy Benefits
If a dependent qualifies for CHAMPVA, the Spina Bifida Health Care Benefits Program, or the Children of Women Vietnam Veterans Health Care Benefits Program, they can get prescriptions through their local pharmacy or through VA’s Meds by Mail program.
What Are VA Education and Vocational Training Benefits for Dependents?
VA offers several educational and vocational training benefits to eligible dependents, including Dependents’ Educational Assistance and the Fry Scholarship.
Dependents’ Educational Assistance
The Survivors’ and Dependents’ Educational Assistance (DEA) program is a part of the GI Bill aimed at offering education and training to eligible survivors and dependents of veterans and service members who:
- Died while on active duty; or
- Passed away as a result of a service-connected disability; or
- Are currently permanently and totally disabled due to a service-connected condition(s).
Specifically, DEA benefits are reserved for the dependents of:
- A veteran who is permanently and totally (P&T) disabled due to a service-connected condition; OR a veteran who passed away from a P&T condition that was incurred during or aggravated by military service.
- A veteran who passed away from any cause while living with a service-connected P&T condition.
- An active-duty service member who is currently missing in action (MIA), “captured in the line of duty by a hostile force,” or “forcibly detained or interned in line of duty by a foreign government or power.”
- An active-duty service member who has been deemed permanently and totally disabled by VA, is receiving outpatient care for said disability, and is likely to be discharged from service because of it.
Eligible survivors and dependents can receive educational assistance for up to 36 months. As of February 2026, full-time students taking part in the DEA program receive $1,574.00 each month while completing their coursework.
The Survivors’ and Dependents’ Educational Assistance program allows eligible students enrolled in the following programs to receive assistance from VA:
- College, university, or other school
- Career training, licensing, and certification tests
- On-the-job training or apprenticeships
- Tutorial assistance
- Work study

Fry Scholarship
The Fry Scholarship is an educational benefit that provides up to 36 months of tuition coverage, a housing stipend, and a book allowance to the dependents of service members who died during active duty after 9/11, among others.
Importantly, a dependent cannot benefit from both the Fry Scholarship and DEA at the same time; they will have to choose one. However, these benefits can be used one after the other for a potential total of 48 months of financial assistance.
Transfer of Education Benefits (TEB)
If a veteran meets certain criteria, they may also be able to initiate a Transfer of Education Benefits (TEB) via request to the Department of Defense. This process allows a veteran’s spouse or child to use any unused educational benefits the veteran still has from the Post-9/11 GI Bill.
Qualifying dependents include spouses and children, who can use these transferred benefits to pay for programs like:
- Undergraduate and graduate education
- Non-college degree programs
- Flight training
- On-the-job training and apprenticeships
- And more
Veterans should note that they will likely have to transfer these benefits while still in active service. It may not be possible after separation from service.
Does VA Offer Home Loan Programs for Surviving Spouses?
Yes, surviving spouses may be eligible for VA-backed home loan programs if they obtain a Certificate of Eligibility (COE) to show the lender that they qualify for this benefit. To qualify for a COE as the surviving spouse, at least one of the following must be true about the veteran:
- The veteran is missing in action (MIA).
- The veteran is a prisoner of war (POW).
- The veteran died while in service or from a service-connected condition, and the surviving spouse did not remarry.
- The veteran died while in service or from a service-connected condition, and the surviving spouse did not remarry before they were 57 years old or before December 16, 2003.
- The veteran had been totally disabled and then died, but their disability may not have been the cause of death (in certain situations).
After applying for the COE, surviving spouses must decide on both the type of loan they are looking to get and the private bank or mortgage company that is serving as their lender. From there, the lender will undergo a process of deciding whether the surviving spouse’s loan application should be accepted.
Does VA Offer Life Insurance?
Yes, Family Servicemembers’ Group Life Insurance (FSGLI) offers coverage for the spouse and dependent children of service members covered under full-time Servicemembers’ Group Life Insurance (SGLI).
With FSGLI, spouses can get up to a maximum of $100,000 (which cannot exceed the service member’s SGLI coverage) while dependent children can get up to $10,000 in coverage.
Are There VA Burial Benefits for Dependents?
Yes, certain veterans and their dependents are eligible for burial benefits through VA based on several criteria.
There are two types of burial benefits: the burial itself and compensation for the costs of the burial. Both have specific eligibility requirements and are handled by two different entities within VA:
- National Cemetery Administration (NCA) and
- Veterans Benefits Administration (VBA).
The National Cemetery Scheduling Office handles eligibility for burial in a VA national cemetery, and a determination of eligibility will only be made after a veteran requests a burial.
What Happens if a Veteran Passes Away?
In the event of a veteran’s death, their surviving dependents may become eligible for several prominent survivor benefits, including Dependency and Indemnity Compensation (DIC) or VA Survivors Pension.
VA Survivors Pension for Dependents
VA Survivors Pension offers monthly payments to qualified surviving spouses and unmarried dependent children of wartime veterans who meet certain income and net worth limits set forth by Congress.
Surviving spouses may be eligible for this benefit if they have not remarried after the veteran’s death, and if the deceased veteran did not receive a dishonorable discharge and their service meets at least one of the requirements listed below:
- Entered active duty on or before September 7, 1980, and served at least 90 days on active military service, with at least one day during a covered wartime period; or
- Entered active duty after September 7, 1980, and served at least 24 months or the full period for which they were called or ordered to active duty (with some exceptions), with at least one day during a covered wartime period; or
- Was an officer and started on active duty after October 16, 1981, and had not previously served on active duty for at least 24 months.
Dependent children may be eligible for this benefit if they are unmarried and under the age of 18, under 23 and attending a VA-approved school, or unable to care for themselves due to a disability that happened before age 18.
Dependency and Indemnity Compensation (DIC)
Dependency and Indemnity Compensation (DIC) is a monthly benefit the Department of Veterans Affairs (VA) awards to a surviving spouse or dependent child(ren) of a service member who:
- Died while on active duty, active duty training, or inactive duty training;
- Died from a service-connected condition; or
- Passed away in a non-service-related manner, but who also received disability compensation for a service-connected condition considered totally disabling:
- For a period of at least 10 years prior to death; or
- Since separation from active duty, and for a period of at least five years prior to death; or
- For at least one year prior to death, if they were a former prisoner of war who died after September 30, 1999.
Unfortunately, not everyone who was married to a service member is entitled to DIC. There are certain criteria that both the veteran and the surviving spouse must meet.
VA’s website states that the surviving spouse of a veteran is eligible to receive Dependency and Indemnity Compensation if they:
- Were married to a service member who died “while on active duty, active duty for training, or inactive duty training”; OR
- Were legally married to the veteran before January 1, 1957; OR
- Married the veteran within 15 years of military discharge when the service-connected condition that caused the veteran’s death began or was aggravated; OR
- Were married to the veteran for at least one year immediately preceding the veteran’s death; OR
- Had a child or children with the veteran, AND
- Continuously cohabited (lived with) the veteran until their time of passing, AND
- Were not separated from the veteran, or, if separated, were not responsible for the separation, AND
- Are not currently remarried.
DIC benefits can be awarded to non-spouses as long as the individual had a child with the veteran and cohabited with them until the time of the veteran’s passing. There are other exceptions to the criteria surviving spouses must meet in order to receive DIC benefits; these exceptions pertain to spousal remarriage and DIC eligibility.
Did VA Make a Mistake with Your Dependent Benefits? Contact CCK Law
If VA denied you dependent benefits you believe you are entitled to or made a different incorrect decision, such as the wrong start date (“effective date”) for benefits, then the representatives at CCK Law may be able to assist. Our dedicated team of attorneys has represented over 36,000 veterans and dependents, helping to secure over $1 billion in wrongfully denied compensation.
Contact CCK Law at 800-544-9144 or contact us online for a free case evaluation.
About the Author
Share this Post