VA Ratings for Migraines Secondary to Depression

CCK Law: Our Vital Role in Veterans Law
Depression can often manifest several secondary conditions, one of those being migraines. Veterans with depression may experience debilitating headaches and therefore it is important to understand how the two conditions are linked.
What are Migraine Headaches?
Migraines are a form of headache that can last for many hours and often interfere with many veterans’ lives. This type of intense headache can bring pain, nausea, vomiting, sensitivity to light and sound, lightheadedness, and blurred vision. Migraines can also create a throbbing sensation on either side of the head. Sometimes an aura, which is categorized by visual disturbances such as flashes of light, may come before a migraine.
There is no singular, definitive cause of migraines, but triggers are thought to include hormonal imbalance, alcohol, stress, sensory stimulation, certain foods, and changes in environment. Medication may be used to treat migraines, as well as rest, diet modification, and stress management. Avoiding triggering stimuli may also help reduce migraines.
Migraines Among Veterans
Migraines are a very common condition among veterans. Studies indicate that veterans are more likely to develop migraines than civilians. Additionally, 36 percent of veterans who served with a one-year deployment to Iraq displayed migraines or signs of migraines.
Some factors which may contribute to the higher rate of migraines among veterans include noise exposure, intense or stressful situations, and traumatic brain injury. Traumatic brain injury (TBI) is caused by a severe blow to the head or injury that penetrates the brain. Migraines are a common side effect of traumatic brain injury.

What is Depression?
Depression is a mental health condition that can interfere with necessary activities in life, such as eating, sleeping, and working, and can affect how a person feels and thinks. Along with migraines, the following are some examples of common symptoms of depression:
- Feelings of sadness, fatigue, worthlessness, guilt, or hopelessness
- Loss of interest or pleasure in usual activities
- Disturbances in sleep
- Anxiety or restlessness
- Irritability
- Difficulty concentrating or remembering things
- Loss of appetite and weight loss or increased appetite and weight gain
- Thoughts of death or suicide
Depression Among Veterans
Like migraines, rates of depression are particularly high among veterans. There are several theories as to why this is, but it is important to note that veterans, especially those who served in combat, experience greater rates of trauma and stress than non-veterans. Specifically, research has also shown that Vietnam Veterans are twice as likely to have elevated depression when compared to WWII Veterans or Korean War Veterans. Thirty percent of active duty and reserve military personnel who served in Iraq and Afghanistan were noted to be experiencing mental health conditions requiring treatment, such as PTSD and depression.
Depression is a serious condition that can cause thoughts of suicide in many veterans. Approximately twenty-two veterans die by suicide every day. Specifically, female veterans are more than 250 percent more likely to commit suicide than their civilian counterparts. Military sexual trauma is regarded as one of the potential reasons the rates of depression and suicide are so high among female veterans. Further potential causes of depression among veterans include exposure to combat, stress, trauma, and separation from one’s home and loved ones.

Relationship Between Migraines and Depression
Research into the relationship between migraines and depression has indicated that people who experience migraines are five times more likely to develop depression than those who do not experience migraines. Migraines are a chronic condition and can often cause a significant amount of recurring pain. Experiencing migraines routinely can cause a person to feel angry, sad, or defeated and may lead to depression.
Conversely, people who have depression may begin to experience migraines. In this case, the depression is not a response to the migraines, but rather the migraines occur as a symptom of depression. This can happen after a person has been living with depression for some time. Anxiety caused by migraines, such as worrying about when the next migraine attack may occur, can also exacerbate depression and depression symptoms.
Service Connection for Migraines and Depression
To establish service connection for migraines or depression, the veteran generally must produce three things:
- A current diagnosis of migraines or depression;
- An in-service incident, injury, or event that caused or aggravated the migraines or depression; and
- A medical nexus linking the current, diagnosed migraines or depression to the in-service occurrence.
Importantly, the veteran does not need to have an official diagnosis of migraines or depression during service to be eligible for service connection. The veteran may be diagnosed after service and still receive a grant of service connection, so long as they can indicate that the migraines or depression are related to service. A medical opinion is often the most successful way to establish the link between the condition and service.
What is Secondary Service Connection?
Secondary service connection is a method of service connection for a disability that has been caused by a condition that is already service-connected. The most crucial part of establishing secondary service connection is providing a nexus.
A nexus is a medical opinion that links a veteran’s secondary disability to the disability that is already service-connected. In order to be granted secondary service connection, there must be a medical nexus that clearly establishes the connection between the primary condition or disability and the secondary condition or disability.
To file a claim for secondary service connection, veterans may file VA Form 21-526, the same as if the veteran were filing for service connection. Veterans will want to be sure they indicate on the form that they are filing for secondary service connection and include all the necessary evidence, such as the diagnosis, medical nexus, and any lay statements to establish the in-service occurrence or explain how the secondary condition was caused by the original service-connected condition.
Secondary Service Connection: Migraines Secondary to Depression
In the instance of migraines and depression, migraines may be claimed as a secondary condition to depression. To be eligible for secondary service connection for migraines, the veteran would need to:
- Already be service-connected for depression;
- Provide a diagnosis for the secondary condition (migraines); and
- Provide medical evidence, or a nexus, showing the relationship between depression and migraines
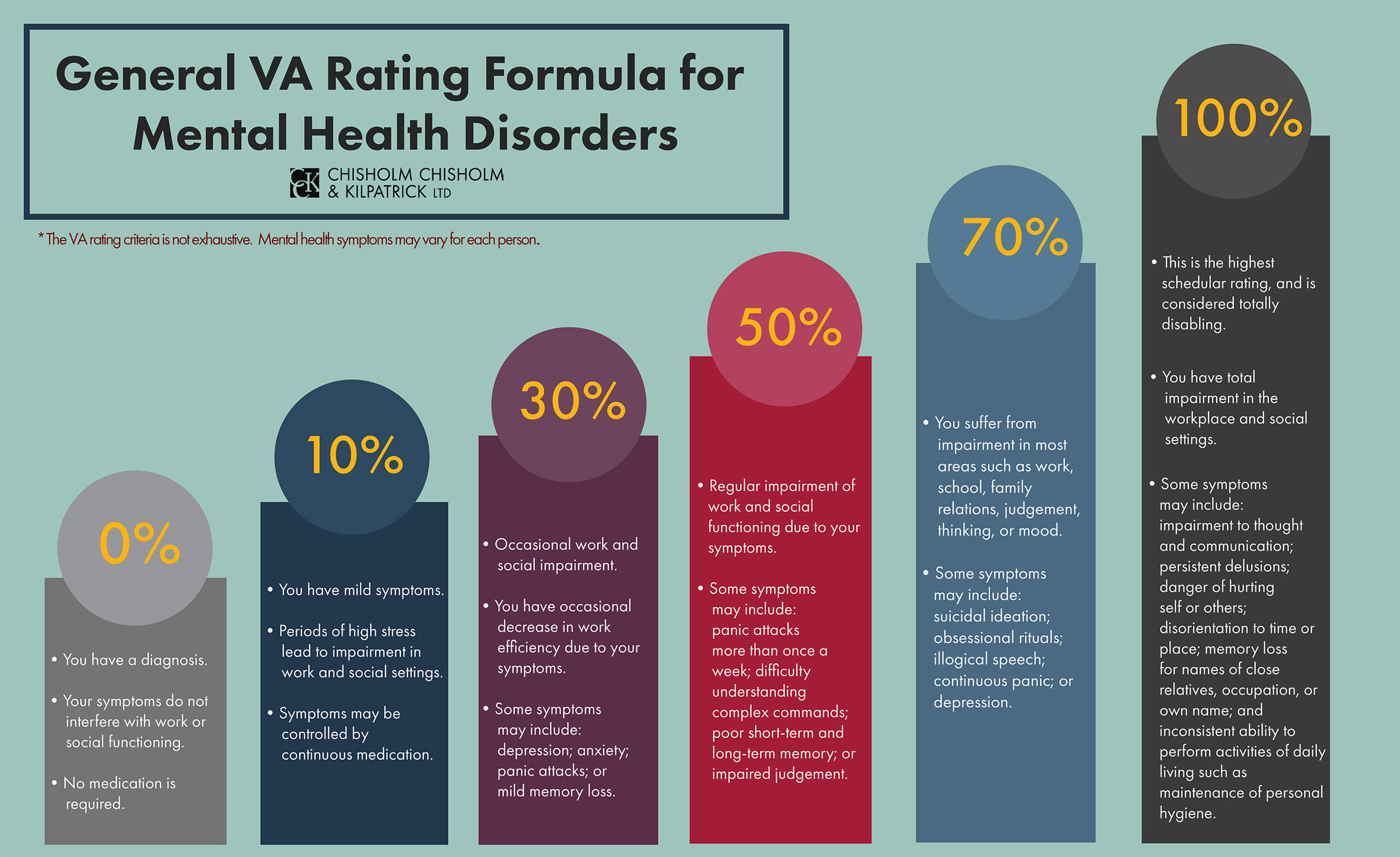
Veterans who develop migraines as a result of depression should consider this process in order to receive benefits for their migraines. Additionally, research has indicated a relationship between migraines and anxiety disorders, another mental health condition. Veterans may also be entitled to secondary service connection if they developed migraines as a result of an anxiety disorder. Below is information regarding how VA rates mental health disorders, such as depression and anxiety.
About the Author
Share this Post