Getting Long-Term Disability (LTD) Benefits for Skin Disorders

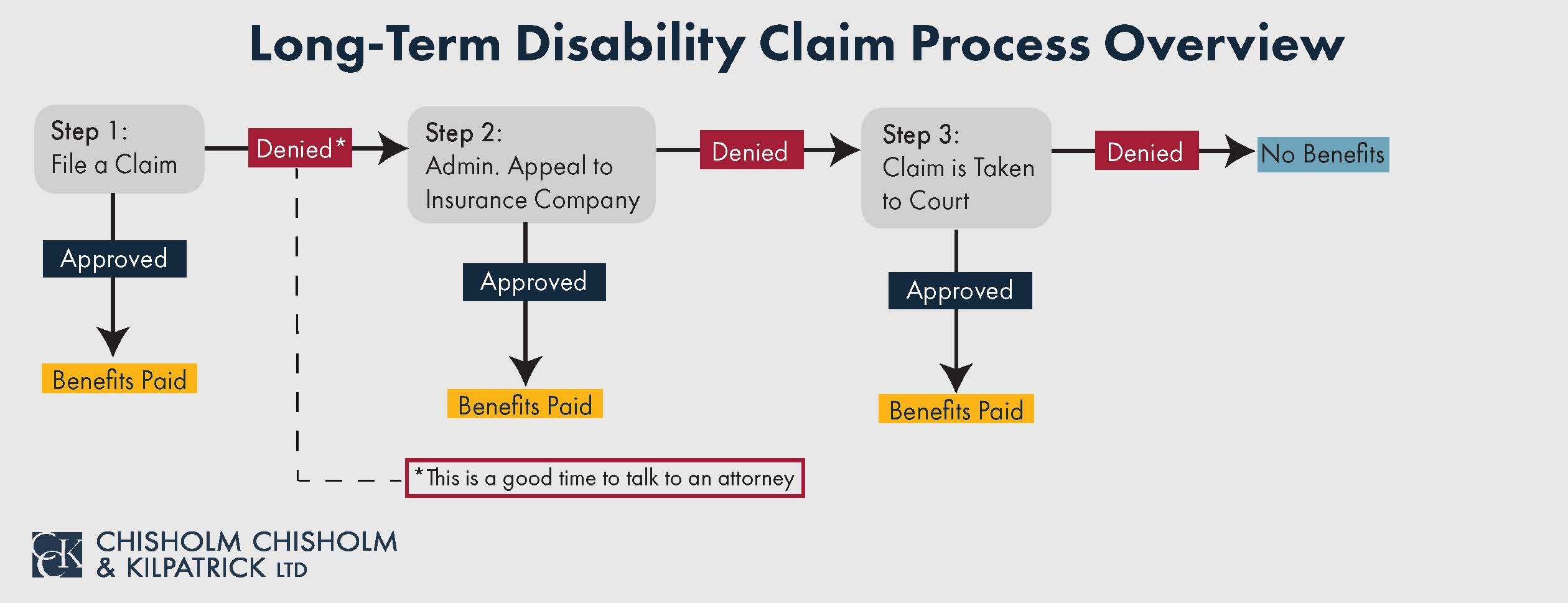
Trying to work with a new and disabling skin disorder can be stressful and you may be wondering what options are available to you should you become unable to work. The process for filing a long-term disability (LTD) claim can be daunting, and many people are unaware of all the evidence they will need to provide in order to receive the benefits to which they are entitled. As a result, wrongful denials by the insurance company are common and leave claimants without the benefits they need to support their families.
At Chisholm Chisholm & Kilpatrick LTD, our team of attorneys and professionals can help you navigate the difficult process of applying for long-term disability benefits and advocate against the insurance company on your behalf. We have experience helping clients at both the initial claim level and the appeal stage and will work to get you the benefits you deserve.
Call us today at 401-331-6300 for a complimentary consultation.
Understanding Skin Disorders
Skin disorders can be more than a cosmetic nuisance. They can also lead to serious disabilities that have long-term health implications. If your chronic skin disorder impairs your ability to work, you may qualify for long-term disability insurance benefits. Below, we will explore some serious skin disorders that often impact a person’s ability to work.
Long-Term Disability and Bullous Disease
Bullous Disease, also known as Bullous Pemphigoid, is a rare skin disorder that occurs when your immune system attacks the thin layer of tissue just below the outer layer of your skin. As a result, large, fluid-filled blisters will often develop on the lower abdomen, upper thighs, or armpits. While the exact cause of this condition is unknown, it can sometimes be triggered by certain medications, light and radiation therapy, or other medical conditions such as diabetes, rheumatoid arthritis, and multiple sclerosis.

Symptoms of bullous disease include itching skin, usually in the few weeks or months prior to the formation of blister; large blisters, usually along folds or creases in the skin, that do not easily rupture when touched; eczema or a hive-like rash; and small blisters or sores that develop in the mouth or in other mucus membranes. Additionally, the skin surrounding the large blisters sometimes appears more reddish or darker than usual. If you begin to experience any of these symptoms, you should see a doctor as soon as possible. Your doctor will likely order a blood test and a biopsy of the blisters in order to determine the correct diagnosis. Further, it is likely that you will be referred to a dermatologist or ophthalmologist, depending on your symptoms and the location of your blisters.
Treatment of bullous disease is commonly focused on healing the skin and relieving itchiness. Your doctor will likely suggest corticosteroids, such as prednisone; steroid-sparing drugs, which will inhibit your immune system’s production of disease-fighting white blood cells; or other medications that fight inflammation. Additionally, depending on the location of the blisters, you may have to alter some of your daily activities, avoid sun exposure, and dress in loose-fitting clothing to avoid the aggravation of the blisters.
While bullous disease often goes away on its own, or within a few months with the help of treatment, severe cases can sometimes take many years to resolve and even become life-threatening, especially for older patients in poor health. Accordingly, severe cases of bullous disease can interfere with your ability to work on a full-time basis. For example, if you suffer from blisters on your hands or feet, you may have difficulty walking, or experience extreme pain when putting pressure on your feet, as well as have difficulty with grasping and fine manipulation, such as writing and typing.
Further, you could have blisters around your eyes, which could make it difficult to see and concentrate on your job duties. Lastly, people with bullous disease often have small blisters in their mouth, making it difficult to eat and drink. The lack of food and water can lead to increased fatigue, loss of energy, and reduced stamina, which would likely impact your ability to work reliably and consistently, day after day.
Long-Term Disability and Dermatitis
While dermatitis is often a general term that describes any skin irritation, more severe cases can cause swollen, reddened skin; blisters that ooze, crust, or flake off; or significantly itchy and dry skin. There are different types of dermatitis and each presents with different symptoms and looks across different areas of the body. Atopic dermatitis, or eczema, is a red and itchy rash that usually develops where the skin flexes, such as inside the elbows, behind the knees, or on the neck. If the rash is scratched, it can lead to blisters that fill with fluid and crust over. Contact dermatitis is typically the result of encountering an irritant or an allergy. The rash is typically red, itchy, and stinging, and blisters can also develop.

Seborrheic dermatitis is a condition that causes red skin, scaly patches, and dandruff. In infants, this type of dermatitis is commonly known as cradle cap. This condition usually affects oily areas of the body such as the face, chest, and back, and can be a long-term condition with periods of improvement and seasonal flare-ups. Lastly, follicular eczema is usually found in people with darker skin and affects the hair follicles. Typically, the affected skin becomes thickened and the follicles can develop bumps.
The treatment of dermatitis usually depends on the type you have, the cause of the condition, and the severity of your symptoms. In addition to lifestyle changes and home remedies, common treatment methods include corticosteroid creams, gels, or ointments; oral corticosteroids such as prednisone; creams or ointments that impact your immune system and can help reduce inflammation; or phototherapy, which involves exposing the affected areas to controlled amounts of light.
While many of the symptoms of dermatitis can appear mild and often go away on their own or with minimal treatment, severe cases can lead to debilitating symptoms that can affect a person’s ability to work. For example, the rash on the skin can become extremely painful and make you uncomfortable during the day and unable to sleep at night. The pain, compounded with increased fatigue from lack of sleep, can often lead to concentration issues and can distract you from your job duties. Further, if you develop blisters, or scratch your skin so often that you have open wounds, there is a chance it could become infected and lead to further complications and can, although rare, become life-threatening.
Long-Term Disability and Ichthyosis
Ichthyosis Vulgaris, also known as fish scale disease, is a skin disorder that causes dead skin cells to accumulate in thick, dry, scales on the skin’s surface. This is an inherited skin disorder that typically presents during early childhood. Most cases of ichthyosis are mild and are often misdiagnosed as severely dry skin. However, sometimes ichthyosis can be severe or complicated by or associated with other conditions such as eczema.

Ichthyosis slows the skin’s natural shedding, which leads to excessive buildup of keratin, a protein found in the upper layer of the skin. Common symptoms of this skin disorder include dry, scaly skin; white, dirty gray, or brown scales; flaky scalp; and deep, painful cracks in the skin. The scales can usually be found on the elbows and lower legs, specifically the shins. While the condition is chronic, the severity of the symptoms usually increases in cold, dry environments and tends to improve in warm, more humid environments. Unfortunately, there is no cure for ichthyosis and treatment revolves around symptom management. In addition to home remedies such as taking long, soaking baths, having a portable home humidifier, and using a pumice stone to help remove the scales, a doctor may prescribe exfoliating creams and ointments or oral medication to help reduce the production of skin cells.
Not only can ichthyosis be embarrassing and make it difficult to concentrate on your job duties, but the cracks in the skin can also be painful and, depending on the location, impact your ability to stand, sit, or walk for extended periods of time. You may find that is difficult to get comfortable in any position, which could also interfere with your sleep and cause increased fatigue during the day. Additionally, having deep cracks or splits in the skin can lead to infections, which can lead to further complications and be life-threatening. Lastly, although rare, ichthyosis can lead to overheating since the thickness of the scales can interfere with a person’s ability to sweat. Alternatively, increased sweating can occur in some people, leading to further embarrassment and distraction during the day.
How CCK Can Help With Your Long-Term Disability Claim for a Skin Disorder
At CCK, we understand how the severity of your skin disorder can impact your ability to work on a full-time basis, reliably and consistently. We can help you navigate the difficult process of submitting a long-term disability claim and assist with a long-term disability appeal should the insurance company deny or terminate your initial claim. We work to submit strong medical and vocational evidence to the insurance company and, specifically at the appeal level, build the strongest record possible before heading to court. This is especially important in ERISA-governed claims because the administrative appeal is usually the claimant’s last opportunity to get supportive evidence into the record.

Since medical evidence is one of the most important aspects of a long-term disability claim, it is important to have good, supportive doctors who are willing to help you with your claim. Insurance companies, in addition to gathering your medical records, often request forms completed by your doctor. It is important for your doctor to fill these out in a timely and accurate manner. Additionally, it is equally important that your medical records demonstrate how your condition impacts your ability to work.
Before filing a long-term disability claim, you should discuss your condition in detail with your doctors and ensure that they are documenting important details in your medical records such as physical exam findings, limitations they observe (e.g. decreased range of motion), medication changes, and side effects, and your personal account of your symptoms. If necessary, your doctor may also have to write a report or speak with the insurance company on your behalf. The more transparency you have with your doctor, the more information they will likely be able to provide to the insurance company.
While handling an LTD appeal, we use our knowledge and expertise regarding ERISA, the U.S. Department of Labor Regulations, and various insurance policies in order to identify any errors the insurance company may have made while handling your claim. We request and review the insurance company’s claim file, the plan governing documents, and the denial letter to develop an appeal strategy that demonstrates your inability to return to work. As part of our strategy, we will gather supportive evidence such as your medical records, reports from your treating doctors, outside expert opinions, and witness statements from you and your family, friends, or co-workers.
Once we gather all the evidence we will need in court, we write a comprehensive appeal that explains why you meet the definition of disability under the policy and are entitled to LTD benefits. Our appeal arguments incorporate both the evidence we gathered and any mistakes made by the insurance company. Call us today at 401-331-6300 for a FREE consultation to see if we can assist you.
Share this Post