Radiculopathy VA Disability Ratings and Benefits

CCK Law: Our Vital Role in Veterans Law
Radiculopathy occurs when a nerve root in the spinal column is pinched and becomes inflamed, causing pain and discomfort. The symptoms and location can vary, and the particular area and nerve affected can impact a veteran’s VA disability rating for radiculopathy.
What Is Radiculopathy?
Radiculopathy is caused by a pinched nerve root in either the cervical, thoracic, or lumbar spine. The pinched nerve can cause pain and discomfort for veterans who experience it, and the pain is often experienced as numbness, tingling, or weakness.
This condition is commonly caused by back conditions such as herniated discs, stenosis, and bone spurs.
Symptoms
- Numbness radiating from the spinal area
- Physical weakness or pain
- Tingling from the spinal area outward into the hips, legs, shoulders, or arms
- General or localized neck or back pain
- Muscle spasms
Types of Radiculopathy
Cervical Radiculopathy
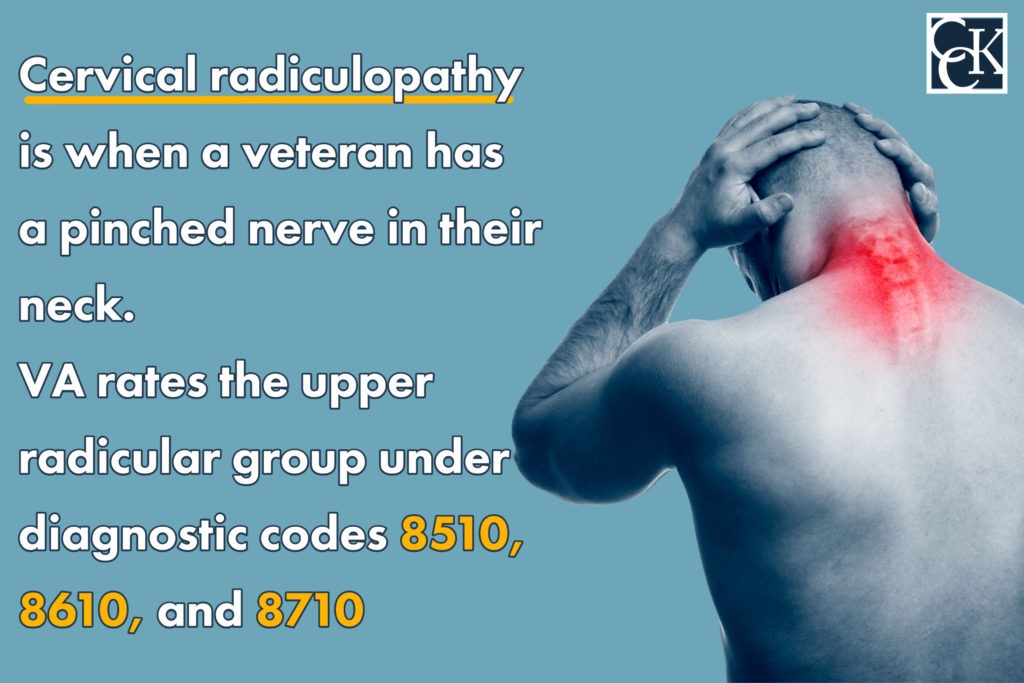
Cervical radiculopathy is when a veteran has a pinched nerve in their neck. When there is pressure on a nerve in the neck, a veteran can experience radiculopathy in their shoulders, arms, hands, and fingers. The type of pain can vary from numbness, tingling or burning, and can also range in severity from mild to severe.
Thoracic Radiculopathy
Thoracic radiculopathy occurs when a nerve in the upper back is pinched, and people may experience pain in their chest or torso area. This is the least common type.
Lumbar Radiculopathy
Lumbar radiculopathy is a common condition among veterans. This occurs when a nerve in the lower portion of the back is pinched, and it can cause numbness and tingling in the hips and legs. Incontinence can also occur as a result.
VA Service Connection for Radiculopathy
To prove service-connection for radiculopathy, a veteran must show a current medical diagnosis of radiculopathy that is linked to the in-service occurrence of the radiculopathy, or an in-service incident that caused or aggravated the radiculopathy.
Examples of in-service incidents may include:
- Breaking or dislocating a vertebra or suffering physical back strain while training
- Operating a weapon
- Lifting equipment
- Jumping
- Completing other military exercises
Veterans do not necessarily need to trace their radiculopathy to one single active-duty incident.

Secondary Service Connection for Radiculopathy
Given that radiculopathy is commonly caused by back conditions, it is typically service-connected on a secondary basis. Secondary service connection is when a veteran’s service-connected condition causes or aggravates a non-service-connected condition, and VA then grants service connection for the secondary condition.
Radiculopathy is a great example of secondary service connection. For example, a veteran is service-connected for degenerative disc disease of the lumbar spine. However, a few years after he was granted service connection, he was diagnosed with radiculopathy of his lower extremities due to his service-connected degenerative disc disease. He can now file a claim with VA for secondary service connection for his radiculopathy since it was caused by his degenerative disc disease.
Radiculopathy is often caused by:
- Back strain or spinal injury
- Degenerative arthritis
- Degenerative disc disease
- Herniated discs
- Spinal stenosis
Secondary conditions are rated in the same manner as primary service-connected conditions, using the same rating schedules.
Service Connection Through Aggravation
In addition to secondary service connection, veterans may also be able to seek service connection through aggravation.
A preexisting condition is presumed “aggravated” if the condition:
- Was noted in the service person’s entrance examination
- Got worse during the person’s time of service, as shown by medical records such as a comparison of reports on the veteran’s disability before and during, or soon after, service
- Worsened more in service than it would have worsened outside of service
- Worsened permanently
A veteran does not need to show that a certain incident during service aggravated the disability—only that it became worse during service.
Aggravation ratings work slightly differently than primary and secondary service connection ratings, depending on the initial severity of the condition compared to the present level of severity.
VA Ratings for Radiculopathy
The diagnostic code used to rate a veteran’s radiculopathy depends on which of the veteran’s nerves are impacted and their level of functioning. Generally, VA measures severity by first determining if the veteran suffers from:
- Paralysis—the nerve cannot function through either complete paralysis or partial paralysis.
- Neuritis—the nerve is still functioning but is swollen, painful, and irritated. Neuritis will require at least one of three things: decreased ability to sense; muscle atrophy; or loss of reflexes.
- Neuralgia—when the nerve causes constant or occasional pain, often characterized by numbness or tingling.
However, symptoms often overlap, and evaluations of paralysis, neuritis, and neuralgia can be confusing and inconsistent.
VA then assigns a rating based on the levels of functioning and severity, and the affected nerve group. Different groups will have different diagnostic codes.

Breaking Down the Nerve Groups
Under these characterizations, each nerve has its own disability rating for each level of severity.
Cervical Radiculopathy
Those with cervical radiculopathy will be rated within the upper radicular group, middle radicular group, and lower radicular group which include the musculospiral nerve, median nerve, axillary nerve, the musculocutaneous nerve, the long thoracic nerve, and the ulnar nerve.
The upper radicular group is rated under diagnostic codes 8510, 8610, and 8710.
Lumbar Radiculopathy
Those with lumbar radiculopathy will be rated within the group of peripheral nerves of the low back and legs. The most commonly affected nerve for this type is the sciatic nerve, which is broken up into five separate nerves depending on which part of the leg is impacted. However, the most common rating for lumbar radiculopathy is under the sciatic nerve.
The sciatic nerve is rated under diagnostic codes 8520, 8620, and 8720.
VA Ratings for Cervical and Lumbar Radiculopathy
If the veteran has objective signs of impairment that can be found via testing, they will get only a moderate rating. The moderate nerve rating changes based on the specific nerve.
Most veterans receive a rating of 10 to 20 percent. Higher ratings are reserved for more severe cases.
The Bilateral Factor
If a nerve condition affects both sides of the body (such as both arms or legs), VA should issue a rating for each side and an additional bilateral factor.
The bilateral factor refers to when a veteran has a disability that affects both arms, both legs, or paired skeletal muscles. In these instances, the ratings will be combined, for the left and right sides, and 10 percent will be added.
The bilateral factor recognizes the limitations caused by these disabilities and how they can impact the veteran.
Refer to our disability calculator to figure out your estimated VA rating.
Was your VA Disability Claim Denied?
The VA disability appeals process is often long and arduous. The skilled attorneys at Chisholm Chisholm & Kilpatrick LTD may be able to help you navigate it. Contact our office for a free case evaluation today at 800-544-9144.
About the Author
Share this Post