Psoriasis VA Disability Ratings and Benefits Explained

CCK Law: Our Vital Role in Veterans Law
What is Psoriasis?
Psoriasis is a common skin condition that is categorized as an immune-mediated disease, meaning it is caused by dysfunction of the immune system. Psoriasis can cause swelling in the body as well as raised plaques or scaly patches on the skin.
An overactive immune system can increase the speed of skin cell growth. Usually, skin cells grow and die off monthly. With psoriasis, skin cells can do this in as little as three or four days. However, once the cells die, they do not shed, but rather stay on the surface of the skin. This is what creates the psoriasis plaques or patches. These patches can be extremely itchy, as well as have a burning or stinging sensation. Psoriasis can occur anywhere on the body, but commonly affects the back of the knees, crook of the elbows, and the scalp.
Symptoms
- Itchiness
- Burning
- Stinging
- Scabs
- Bleeding
- Swollen and stiff joints
Risk Factors
Currently, the exact cause of psoriasis is unknown, although genetics may play a role. Some triggers may aggravate symptoms and worsen the condition. These triggers can include:
- Stress
- Injury, specifically to the skin
- Hormonal changes
- Increased alcohol consumption
- Smoking
- Some medications, such as ibuprofen, ACE inhibitors, and lithium
- Throat infections
- Some weather conditions, such as cold and dry weather
- Additional immune disorders, such as HIV
- Certain exposures
Importantly, psoriasis is not contagious, meaning that it does not spread from person to person. Additionally, psoriasis can cause or aggravate other conditions such as:
- Arthritis
- Eye injections
- Diabetes
- High blood pressure
- Heart disease
- Celiac disease
- Sclerosis
- Crohn’s disease
- Mental health conditions like anxiety and depression
Diagnosing Psoriasis
A dermatologist’s expert opinion may be necessary to diagnose psoriasis. There are multiple forms of psoriasis, meaning that a dermatologist can identify which form of psoriasis a person may have.
Forms of Psoriasis
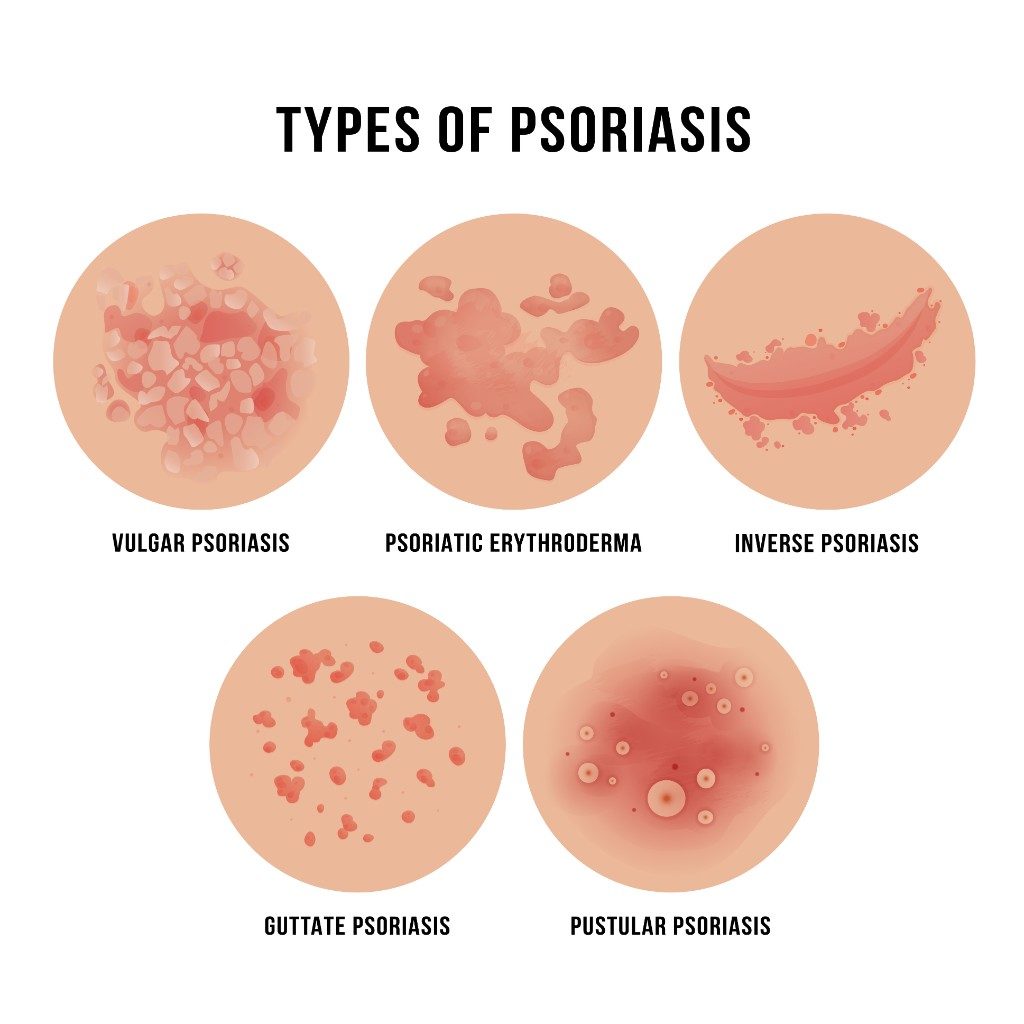
- Plaque Psoriasis—This type of psoriasis is most common, and affects around 80 percent of people with psoriasis. Plaques, or scaly raised patches, can form anywhere on the body and commonly in the knees, elbows, and scalp.
- Guttate Psoriasis—Guttate psoriasis can occur after an infection of strep throat. A person may develop papules, or round spots that are raised. They can appear on the arms, legs, torso, face, ears, and scalp.
- Inverse Psoriasis—People diagnosed with inverse psoriasis often have smooth skin, as opposed to the scaly, raised bumps typical of psoriasis. The smooth skin may be inflamed and reddened. This form usually occurs in folds in the skin, like the underarm areas and genitals. Inverse psoriasis is often very itchy and painful and worsened by sweat.
- Pustular Psoriasis—This form of psoriasis is categized by pustules, or pus-filled bumps, which may be surrounded by swollen or reddened skin.
- Erythrodermic Psoriasis—A rarer form of psoriasis, erythrodermic psoriasis can cause the skin to shed in large sheets. It usually affects the whole body and can cause severe itching, changes in heart rate, and nail changes.
Treating Psoriasis
There are multiple methods of treatment which may be used to treat psoriasis and alleviate symptoms. Such treatment can include:
- Topical treatments—Topical treatments like creams and ointments can be applied directly to the skin to alleviate itch, swelling, and pain.
- Phototherapy—Light therapy which can use ultraviolet light to treat the skin.
- Systemic treatment—Oral medications or injections which can work throughout the whole body.

How Do I Get VA Service Connection for Psoriasis?
There are multiple methods by which to establish service connection for psoriasis, including directly, secondarily, or presumptively.
Direct Service Connection for Psoriasis
Direct service connection is when a veteran proves to VA that an in-service event of some kind directly caused or worsened the veteran’s condition. To be granted direct VA service connection for psoriasis, veterans must establish the following key elements of service connection:
- An in-service event, injury, or illness;
- A current diagnosis of psoriasis by a medical professional; and
- A medical nexus, or link, between your in-service event, injury, or illness and your current diagnosis.
Secondary Service Connection for Psoriasis
Secondary service connection can be achieved if a veteran’s psoriasis was developed as a result of a separate service-connected condition. For example:
- Say a veteran was exposed to toxic chemicals during their military service, eventually causing them to develop hypothyroidism. VA recognizes that the veteran’s thyroid condition is service connected and grants them a VA rating for hypothyroidism.
- Over time, the veteran’s thyroid condition causes other symptoms to crop up in their body, including psoriasis. The veteran’s physician offers their opinion that the veteran’s thyroid condition was a potential trigger for this newfound psoriasis.
- In this situation, the veteran may be able to pursue a VA claim for psoriasis secondary to hypothyroidism, since their primary service-connected condition (hypothyroidism) has now caused a secondary condition to develop (psoriasis).
- If the veteran’s claim is successful, they may be awarded a VA rating and compensation for their psoriasis.
Presumptive Service Connection for Psoriasis
Presumptive conditions are those that VA automatically assumes are connected to a veteran’s military service, depending on the location and timeframe in which they served.
For example, many Vietnam veterans were exposed to the chemical herbicide Agent Orange while deployed during their service, a toxin which is now known to cause negative health effects. Because of this, so long as a veteran can present proof that they served in Vietnam during the qualifying time period, VA may automatically presume that any Agent Orange-related conditions the veteran has developed are a result of their exposure to the chemical.
Unfortunately, as of December 2025, VA has not added psoriasis to its list of presumptive conditions for exposure to either Agent Orange, nor to the PACT Act conditions for military burn pits in the Middle East. This means presumptive service connection is off the table for most veterans.
However, because some scientific research has connected toxic exposure to the development of psoriasis, veterans who were exposed to toxic chemicals during their military service may still be able to cite their exposure while pursuing direct or secondary service connection for their condition.

Compensation and Pension (C&P) Exams for Psoriasis
Once a claim has been filed, VA may request a Compensation and Pension exam, or C&P exam. This exam will usually be performed by a VA physician or VA contracted physician who may physically examine the veteran, as well as ask questions regarding the veteran’s military service, their psoriasis, or symptoms of their psoriasis.
To schedule a C&P exam, VA will usually call the veteran or send them a letter. As such, it is crucial to ensure that VA has the veteran’s most up-to-date contact information. If VA does not have the current contact information, the veteran might miss a C&P request. Failure to attend an exam, or to reschedule a missed exam, could result in the denial of a veteran’s claim.
Prior to the exam, the examiner should review the veteran’s c-file. The c-file will usually contain any documentation that has previously been submitted to VA, as well as the veteran’s medical and military service records.
The veteran may also use a DBQ, or Disability Benefits Questionnaire, to bolster their claim. A Disability Benefits Questionnaire is a form created by VA so that the veteran may address important aspects of their condition, such as symptoms, severity, possible causes, and relation to other disabilities. The veteran may also have their private doctor fill out a DBQ for them. In the case of psoriasis, a dermatologist who regularly treats the veteran for their psoriasis may fill out a DBQ for the veteran to provide insight to VA.
How Does VA Rate Psoriasis?
VA rates skin conditions under 38 CFR § 4.118, Diagnostic Codes 7800-7833. Psoriasis is listed under Diagnostic Code 7816. Several skin conditions are rated based on the amount of skin that is affected. VA’s rating schedule proposes two ways to determine this: calculations and estimations.
Skin area calculations take into account the surface area in inches squared that is affected whereas skin area estimations take into account the percentage of skin that is affected. However, scars on the head, face, or neck are rated based on skin loss and how many facial features have been disfigured.
On the other hand, disability ratings for scars on areas of the body other than the head, face, or neck are generally based on the size of the scar.
The General Rating Formula for the Skin is included in 38 CFR § 4.118 and is used to rate the majority of skin conditions:
- “60% – at least one of the following: characteristic lesions involving more than 40% of the entire body or more than 40% of exposed areas affected; or constant or near-constant systemic therapy including, but not limited to, corticosteroids, phototherapy, retinoids, biologics, photochemotherapy, psoralen with long-wave ultraviolet-A light (PUVA), or other immunosuppressive drugs required over the past 12-month period
- 30% – at least one of the following: characteristic lesions involving 20-40% of the entire body, or 20-40% of exposed areas affected; or systemic therapy including, but not limited to, corticosteroids, phototherapy, retinoids, biologics, photochemotherapy, PUVA, or other immunosuppressive drugs required for a total duration of 6 weeks or more, but not constantly, over the past 12-month period
- 10% – at least one of the following: characteristic lesions involving at least 5%, but less than 20%, of the entire body affected, or at least 5% but less than 20%, of exposed areas affected, or intermittent systemic therapy including, but not limited to, corticosteroids, phototherapy, retinoids, biologics, photochemotherapy, PUVA, or other immunosuppressive drugs required for a total duration of fewer than 6 weeks over the past 12-month period
- 0% – no more than topical therapy required over the past 12-month period and at least one of the following: characteristic lesions involving less than 5% of the entire body affected; or characteristic lesions involving less than 5% of exposed areas affected; or rate as disfigurement of the head, face, or neck (DC 7800) or scars (DCs 7801, 7802, 7804, or 7805), depending upon the predominant disability”
Here, VA defines systemic therapy as any treatment that is injected, or taken by mouth, through the nose, or anally. This includes, but is not limited to, the treatments listed within the rating criteria. VA defines topical therapy as any treatment applied directly to the skin, regardless of the type of drug.
For psoriasis, any complications that arise from the condition, such as psoriatic arthritis, are rated separately under their appropriate diagnostic code.

Call CCK Today for a Free Case Evaluation With the VA Disability Team at Chisholm Chisholm & Kilpatrick LTD
If you have previously been denied monthly VA disability benefits for your psoriasis, the veterans’ advocates at Chisholm Chisholm & Kilpatrick LTD may be able to assist you. We are committed to helping veterans receive the benefits they deserve. For a free case evaluation, call us today at (800) 544-9144.
About the Author
Share this Post

