VA Disability Ratings for Dysthymia

CCK Law: Our Vital Role in Veterans Law
Dysthymia is a form of depression that can affect many people, especially veterans. If you are a veteran who is experiencing depression or dysthymia, help is available. You may also be eligible for VA disability compensation benefits. Continue reading to learn more.
What is Dysthymia?
Dysthymia is a “milder, but long-lasting form of depression.” Sometimes it is referred to as persistent depressive disorder. Importantly, people who have dysthymia may also experience periods of major depression.
Depression is categorized as a mood disorder, which can affect the body, emotions, and thoughts. Often, people who experience depression, or dysthymia, can have overwhelmingly negative thoughts. These thoughts can interfere with a person’s ability to perform necessary life tasks on a day-to-day basis.
What Causes Dysthymia?
There is not one specific, clear cause for dysthymia, but rather mental health specialists speculate that dysthymia could be linked to chemical imbalances in the brain. There are also environmental, psychological, biological, and genetic factors which could contribute to whether a person is likely to experience dysthymia.
Other factors such as chronic stress or trauma can contribute to a person’s likelihood to experience dysthymia. Dysthymia can also run in families.
Symptoms
Compared to depression, dysthymia symptoms are often milder, but longer lasting. Though individuals may experience different symptoms, some signs may include:
- Feelings of emptiness, sadness, or anxiousness
- Decreased ability to concentrate
- Indecisiveness
- Fatigue or lethargy
- Feelings of hopelessness
- Changes in weight or appetite
- Changes in appearance
- Disturbances in sleep patterns, such as oversleeping or insomnia
- Low self-esteem
Diagnosing Dysthymia
Like depression, dysthymia can usually be diagnosed by a mental health practitioner, such as a psychologist or psychiatrist. A mental health practitioner may also review a person’s medical history to see if there is any correlation with other conditions, since depression can often co-exist with conditions like heart disease or cancer. Dysthymia can also co-exist with substance abuse disorders or anxiety disorders.
Treating Dysthymia
Many of the same methods of treatment that are used for depression are also used to treat this condition. Specifically, there are forms of medication which can be used to treat dysthymia, or depression. Usually, anti-depressants are prescribed.
Another form of treatment which can be considered is therapy. Cognitive behavioral or interpersonal therapy may be helpful to treat the overwhelmingly negative thoughts or feelings a person with dysthymia may experience.
VA Service Connection for Dysthymia
To receive VA disability benefits for dysthymia, veterans experiencing dysthymia first need to establish service connection with VA. To do this, veterans first need to fill out VA Form 21-526EZ, or Application for Disability Compensation and Related Compensation Benefits. In addition, veterans need to submit:
- A current diagnosis of dysthymia; and
- An in-service event, injury, or illness which caused or contributed to the veteran’s dysthymia; and
- A nexus which links the veteran’s dysthymia to their military service
For example, if the veteran experiences dysthymia due to witnessing a traumatic event. If this is the case, the veteran could submit evidence that they witnessed the event, such as a lay statement, and medical evidence linking the trauma of witnessing the event to their dysthymia.

VA Ratings for Mental Disorders
As dysthymia is considered a form of depression, VA rates dysthymia using the same criteria as for depression. Specifically, VA rates all mental health conditions, aside from eating disorders, using VA’s General Rating Formula for Mental Disorders (38 CFR § 4.130). VA may assign a rating ranging from 10 percent to 100 percent using these criteria. The rating will be assigned based on the level of social and occupational impairment the veteran experiences. The criteria are listed below:
- 100% – total occupational and social impairment, due to such symptoms as: gross impairment in thought processes or communication; persistent delusions or hallucinations; grossly inappropriate behavior; persistent danger of hurting self or others; intermittent inability to perform activities of daily living (including maintenance of personal hygiene); disorientation to time or place; memory loss for names of close relatives, own occupation, or own name
- 70% – occupational and social impairment, with deficiencies in most areas, such as work, school, family relations, judgment, thinking, or mood, due to such symptoms as: suicidal ideation; obsessional rituals which interfere with routine activities; speech intermittently illogical, obscure, or irrelevant; near-continuous panic or depression affecting the ability to function independently, appropriately and effectively; impaired impulse control; spatial disorientation; neglect of personal appearance and hygiene; difficulty in adapting to stressful circumstances (including work or a work-like setting); inability to establish and maintain effective relationships
- 50% – occupational and social impairment with reduced reliability and productivity due to such symptoms as: flattened affect, circumstantial, circumlocutory, or stereotyped speech; panic attacks more than once a week; difficulty in understanding complex commands; impairment of short- and long-term memory; impaired judgment; impaired abstract thinking; disturbances of motivation and mood; difficulty in establishing and maintaining effective work and social relationships
- 30% – occupational and social impairment with occasional decrease in work efficiency and intermittent periods of inability to perform occupational tasks (although generally functioning satisfactorily, with routine behavior, self-care, and conversation normal), due to such symptoms as: depressed mood, anxiety, suspiciousness, panic attacks (weekly or less often), chronic sleep impairment, mild memory loss (such as forgetting names, directions, recent events)
- 10% – occupational and social impairment due to mild or transient symptoms which decrease work efficiency and ability to perform occupational tasks only during periods of significant stress, or symptoms controlled by continuous medication
- 0% – a mental condition has been formally diagnosed, but symptoms are not severe enough either to interfere with occupational and social functioning or to require continuous medication
TDIU With Dysthymia
Veterans with dysthymia may also be eligible for a benefit offered by VA called TDIU, or total disability based on individual unemployability. This benefit compensates veterans at the 100 percent rating level, even if their overall combined rating may be less than that. Specifically, veterans can qualify for TDIU in one of two ways:
- Schedular TDIU
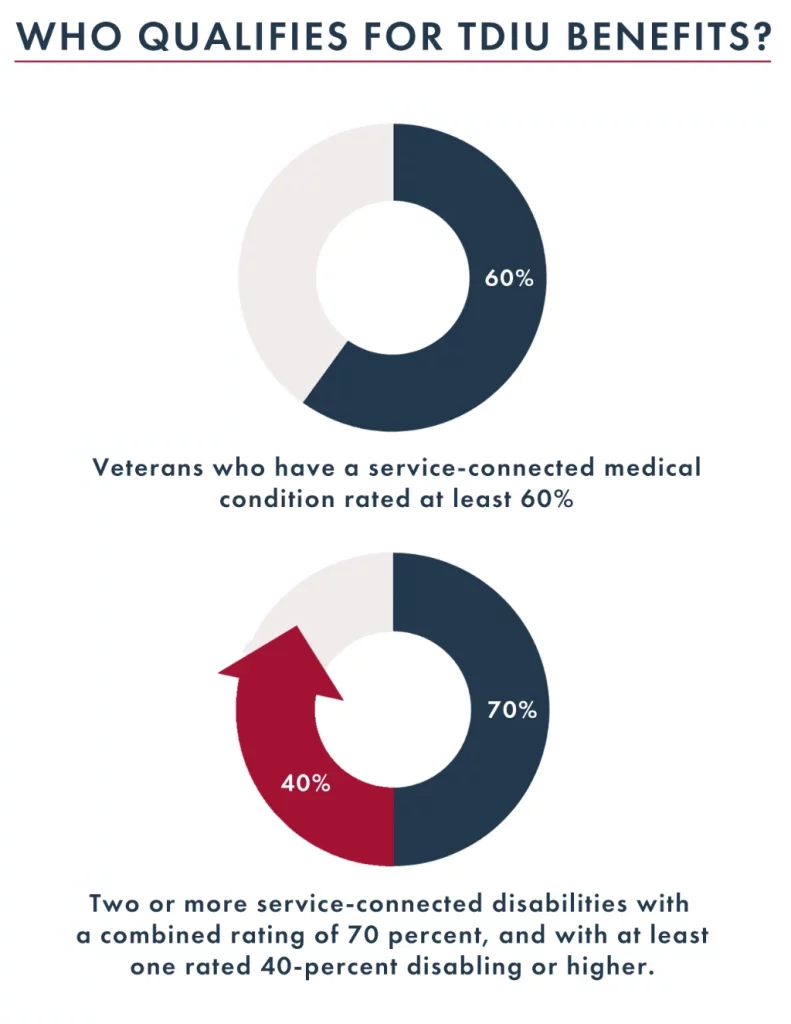
In order to be eligible for Schedular TDIU, veterans must have one condition rated at 60 percent minimum OR two conditions that can be combined to reach 70 percent, where one condition is at minimum 40 percent. The criteria for schedular TDIU is outlined under 38 CFR § 4.16a. Ratings given for dysthymia, or depression can contribute to schedular TDIU eligibility.
- Extraschedular TDIU
Veterans who do not meet the necessary criteria for schedular TDIU may be eligible for extraschedular TDIU. For this form of TDIU, veterans must prove that their condition(s) uniquely hinder their ability to maintain substantially gainful employment. Extraschedular TDIU is rated under 38 CFR § 4.16b.
Need Help with Your Appeal for Dysthymia Benefits?
If you are a veteran who needs assistance fighting your appeal for VA benefits, the accredited representatives at Chisholm Chisholm & Kilpatrick may be able to help. Our veterans’ advocates can craft skilled arguments and gather evidence to help support your case. If you need representation, call our office today for a free case evaluation.
About the Author
Share this Post
