VA Disability Benefits for Bulging Disc

CCK Law: Our Vital Role in Veterans Law
What is a Bulging Disc?
Discs act as cushions between the vertebrae in your spine. They are composed of an outer layer of tough cartilage that surrounds softer cartilage in the center. Discs tend to show signs of wear and tear with age or due to injury. Over time, discs dehydrate and their cartilage stiffens. Those changes can cause the outer layer of the disc to bulge out all the way around its circumference. A bulging disc does not always affect the entire perimeter of a disc, but at least a quarter if not half of the disc’s circumference is usually affected. Only the outer layer of tough cartilage is involved.
A bulging disc may have no pain at all if it has not reached a certain level of severity. This can make it difficult for healthcare providers to identify the bulging disc symptoms before the condition becomes more severe. Most commonly, bulging discs create pressure points on nearby nerves, which create a variety of sensations.
Symptoms may range from mild tingling and numbness to moderate or severe pain. Numbness, tingling, and pain may occur in the fingers, hands, arms, neck, or shoulders. This would most likely indicate a bulging disc in the cervical (i.e., neck) area. However, most individuals with bulging discs have problems occur in the lumbar area. In this case, symptoms may involve pain in the feet, thighs, lower spine, and buttocks. Additionally, such individuals may experience difficulty with walking. In severe cases, bladder incontinence can occur because of a bulging disc compressing the nerves that control the bladder.
A thorough medical examination including X-ray and in some cases, CT or MRI scans are necessary to diagnose bulging disc conditions. Once a diagnosis is made, individuals can usually begin the process of treating their bulging discs. A doctor may recommend physical therapy to strengthen the muscles in the back and to regain lost mobility. Non-surgical treatments are usually successful in managing bulging discs.

Service Connection for Bulging Discs
In order to establish service connection for a bulging disc, veterans must meet a number of requirements. First, they must provide a current diagnosis of their bulging disc from a healthcare provider. From there, they must provide evidence of an in-service event, injury, or illness. The final step is arguably the most important element of service connection and involves providing a medical nexus opinion. Both VA doctors and private health care physicians can provide medical nexus opinions. For a service connection claim to be successful, the nexus opinion must use certain language that matches up with VA’s evidentiary standard. Thus, a positive nexus opinion would have to state that the veteran’s bulging disc is “at least as likely as not” due to their time in service.
How Does VA Rate Bulging Disc
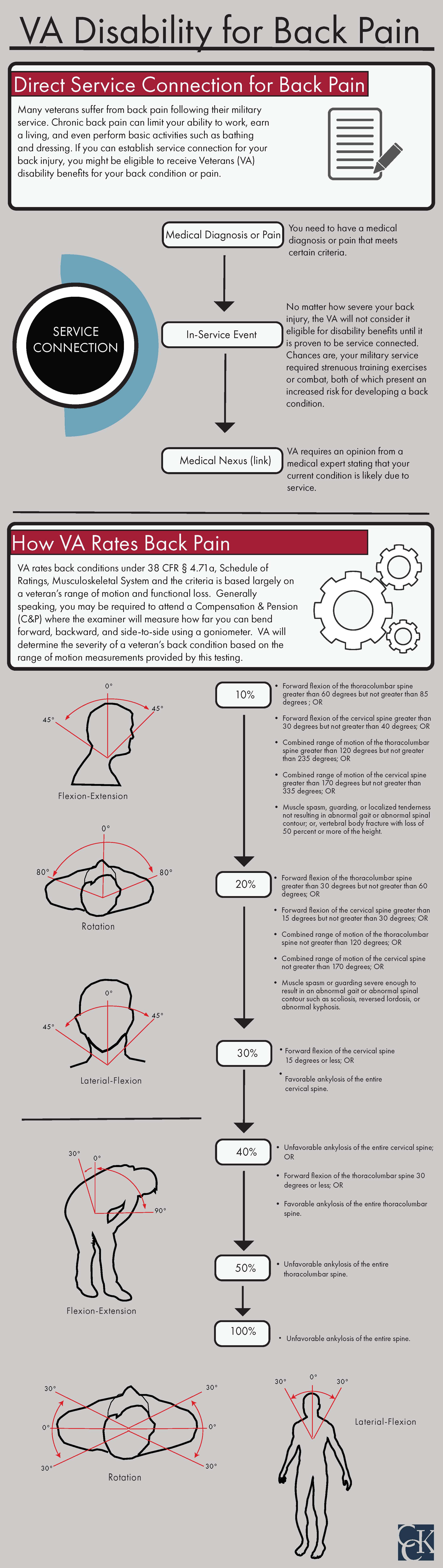
VA rates bulging disc according to 38 CFR § 4.71a, Schedule of Ratings – Musculoskeletal System. Typically, VA uses the General Rating Formula for Disease and Injuries of the Spine, which is largely based on a veteran’s range of motion. Generally speaking, veterans will attend a Compensation & Pension (C&P) examination and the examiner will measure how far they can bend forwards, backwards, and side to side, using a goniometer.
VA will determine the severity of a veteran’s back condition based on the range of motion measurements provided by the examiner. However, the C&P examiner should also take into account the functional loss caused by the veteran’s back condition, as evidenced by pain during motion. For example, a veteran might be able to bend forward 85 degrees, but starts to experience pain at 55 degrees. In this case, the veteran should receive a disability rating that is consistent with both the range of motion measurements and functional limitations caused by their back pain.
It is important to note that for bulging disc, VA may also consider an evaluation under intervertebral disc syndrome if the veteran meets the criteria outlined below:
- 60% – with incapacitating episodes having a total duration of at least 6 weeks during the past 12 months
- 40% – with incapacitating episodes having a total duration of at least 4 weeks but less than 6 weeks during the past 12 months
- 20% – with incapacitating episodes having a total duration of at least 2 weeks but less than 4 weeks during the past 12 months
- 10% – with incapacitating episodes having a total duration of at least one week but less than 2 weeks during the past 12 months
Here, an incapacitating episode is a period of acute signs and symptoms due to intervertebral disc syndrome requires bed rest prescribed by a physician and treatment by a physician. If a veteran’s bulging disc qualifies for either rating formula, VA should use whichever method results in the higher evaluation.
VA Claim for Bulging Disc Denied?
If your bulging disc was caused by service in the military and have been denied benefits for this condition, contact the Veterans (VA) disability attorneys at Chisholm Chisholm & Kilpatrick LTD at (401) 331-6300 for a free consultation.
About the Author
Share this Post