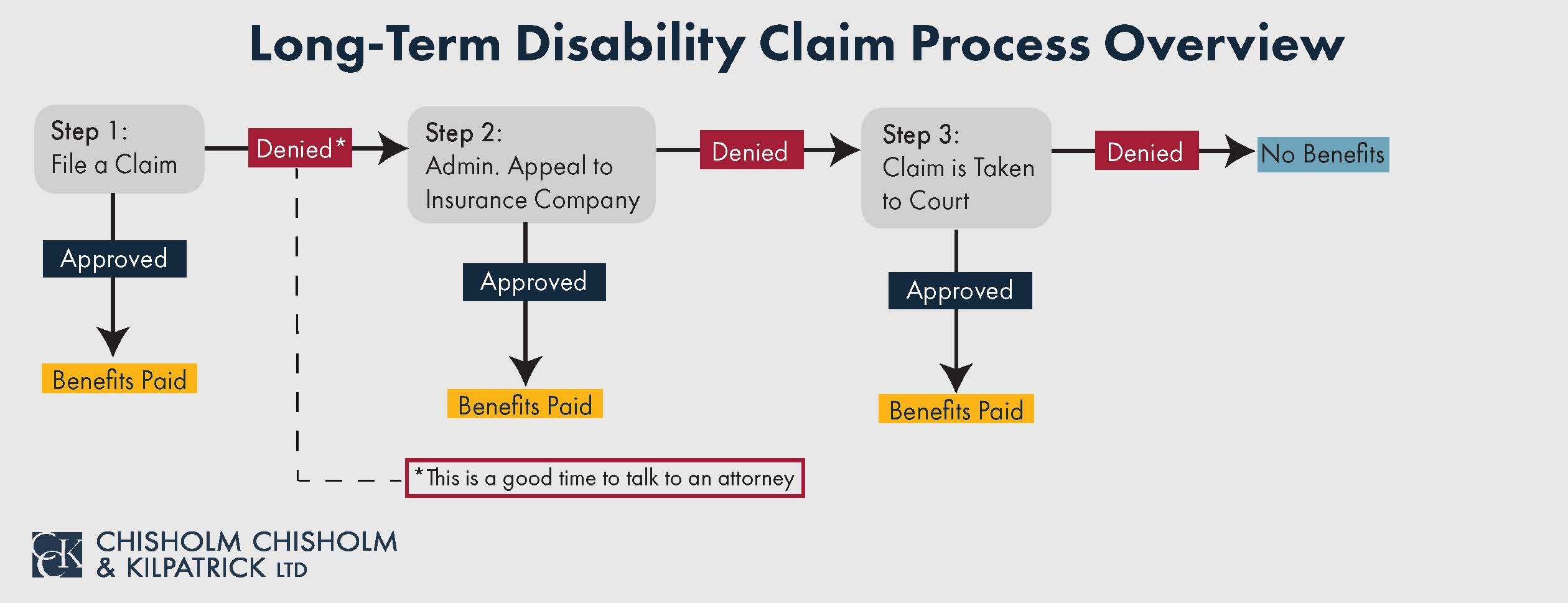
Long-Term Disability (LTD) Insurance Company Deadlines: ERISA

Employer-provided long-term disability (LTD) policies are governed by the Employee Retirement Security Act of 1974 (ERISA), which includes requirements for deadlines. Insurance companies must follow the ERISA regulations when issuing decisions on your long-term disability claim or appeal.
Initial Claim Decision Deadlines
In order to receive long-term disability (LTD) benefits, you will need to file an initial claim with your LTD insurance provider. Once you submit your claim forms and any requested documents, the insurance company has deadlines it must meet to issue a decision. It is important that you read your LTD policy to understand the rules that apply to your claim. Insurance companies’ decision deadlines are often governed by ERISA regulations 29 CFR § 2560.503-1(f)(3) and 29 CFR § 2560.503-1(f)(4). Upon submitting your claim forms, the insurance company has 45 days to issue a decision.

However, the insurance company can take a 30-day extension if it provides notice of the extension in writing. Following this extension, the insurance company can take an additional 30-day extension if a decision has yet to be made. The extension letters must explain the standard to which entitlement to a benefit is based, the unresolved issues that prevent a decision on the claim, and the additional information needed to resolve those issues.
If the insurance company takes an extension because you did not supply the information necessary to decide the claim, the time period to make a decision is tolled and the extension period will not begin until that information is received. The circumstances of your claim can impact the deadlines that the insurance company must meet. You should consider contacting an attorney if the deadline for a decision has passed and you have not heard from your insurance company.
Appeal Decision Deadlines
If your LTD claim is denied or your benefits are terminated, you need to file an administrative appeal with the insurance company. When an ERISA-governed long-term disability claim is denied, the appeal decision deadlines are specifically governed by 29 CFR § 2560.503-1(i)(1)(i), 29 CFR § 2560.503-1(i)(3)(i), and 29 CFR § 2560.503-1(i)(4). Once you submit your appeal, the insurance company has 45 days to issue a decision. However, the insurance company can take an additional 45-day extension if it determines that special circumstances require additional time to process the appeal.

As with initial claims, an extension notice for an appeal must be sent to you in writing. In the letter, the insurance company must explain the special circumstances requiring an extension of time and include the date by which they expect to issue a decision. You should carefully examine the special circumstance(s) noted by the insurance company to ensure that an extension is, in fact, warranted; if it is not, you may want to challenge the asserted necessity of the extension.
Additionally, like initial claims, if the insurance company takes an extension because you did not supply information necessary to make a decision on the appeal, the time period to make a decision is tolled and the 45-day extension period will not begin until that information is received. You should contact an attorney if you disagree with the special circumstances proposed by the insurance company or if the appeal decision deadline has passed without an update from the insurance company.
Contact CCK for Denied Long-Term Disability Claims
At Chisholm Chisholm & Kilpatrick LTD, our team of attorneys and professionals have experience holding insurance companies accountable to deadlines and the terms of the policies they issue. We understand that extensions can cause increased financial hardship. We can help you to assemble a strong claim or appeal and make sure that the insurance company issues a decision in a timely manner. Contact us now at (401) 237-6412 for a FREE consultation to see if an ERISA lawyer can help. We look forward to speaking with you.
About the Author
Share this Post